Strongyloidiasis
Alerts and Notices
Important News & Links
Synopsis

S stercoralis follows a complicated life cycle; after skin penetration, larvae migrate through the body and eventually reach the intestine where they either develop into adult nematodes and lay eggs or remain as infective larvae. The eggs are excreted in stool and the larvae migrate to the perianal skin and cause the cutaneous manifestations. Autoinfection may also occur, whereby the larvae migrate to the lungs, are coughed up and swallowed, and re-infect the intestinal tract.
The infection may remain quiescent for years and it is commonly asymptomatic in immunocompetent individuals. Acute infection may present with GI or pulmonary symptoms, if any. Symptoms of chronic infection may be specific (larva currens) or nonspecific (chronic abdominal pain, intermittent diarrhea, chronic urticaria / angioedema, nausea, constipation, coughing / wheezing, prurigo nodularis, or rarely, reactive arthritis).
Larva currens is an urticarial, pruritic, and sometimes painful eruption that starts at the perianal area and spreads quickly to involve the buttocks, thighs, and abdomen. It appears as 1 or more linear or serpiginous erythematous plaques. Each linear plaque extends at a rate of 5-15 cm/hr, hence the name larva currens. Larva currens lasts hours to days but may recur in the setting of autoinfection.
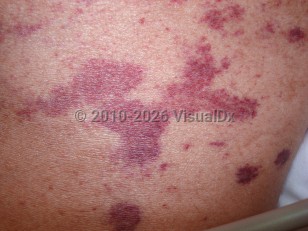
In immunocompromised patients, hyperinfection syndrome may occur, resulting in massive worm burden, which causes organ invasion, sepsis or septic shock, meningitis associated with intestinal bacteria, and death (70%-90% mortality rate). Hyperinfection syndrome manifests as "thumbprint purpura:" rapidly progressing purpura, including retiform purpura and petechiae that radiate out from the periumbilical area. This is caused by dermal invasion of large numbers of larvae that results in vascular occlusion.
Immunocompromised patients who are especially susceptible to hyperinfection include those on concurrent systemic corticosteroids or vincristine, those with AIDS, malnutrition, hematologic malignancy, solid organ or hematopoietic stem cell transplant recipients, or human T-cell lymphotropic virus type 1 (HTLV-1) infection. Transplant recipients with graft-versus-host disease (GVHD) are at an especially high risk due to concurrent corticosteroid treatment of GVHD.
Risk factors include gardening, farming, having a psychiatric illness / being a long-term psychiatric patient (poor sanitation and pica), travel to hyperendemic areas, low socioeconomic status, being a prisoner of war, and walking barefoot outdoors. There are also multiple reports of transmission from an infected donor organ.
Symptoms may persist for weeks to decades and may be frequent or lie quiescent for months at a time. The longest documented infection is 65 years.
Codes
B78.1 – Cutaneous strongyloidiasis
SNOMEDCT:
240855004 – Cutaneous strongyloidiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/30/2022
 Patient Information for Strongyloidiasis
Patient Information for Strongyloidiasis - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient