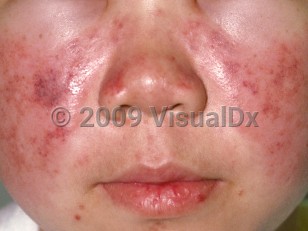
Systemic lupus erythematosus in Child
See also in: Nail and Distal DigitAlerts and Notices
Important News & Links
Synopsis

This summary discusses systemic lupus erythematosus in children. Neonatal lupus erythematosus is addressed separately.
Systemic lupus erythematosus (SLE) is a disease of unclear etiology characterized by immune abnormalities and multiorgan involvement. Approximately 15%-20% of patients with SLE will present during the first 2 decades of life. Childhood-onset SLE is a phenotype of SLE that presents in childhood or adolescence. It is relatively rare, with a worldwide prevalence estimated at 1.89-25.7 per 100 000 children. On average, it presents with a more aggressive phenotype than adult-onset SLE. Constitutional symptoms, fever, fatigue, anemia, weight loss, headache, mood disturbances, arthralgias, and skin findings may all be seen. Fatigue and weight loss may be exacerbated by generalized nutritional complications associated with SLE and can sometimes be extreme. Choreiform movements may occur. Neurologic and renal involvement is a prominent characteristic in childhood SLE and often portends greater disease morbidity. Childhood SLE is also associated with chronic cardiopulmonary disease and macrophage activation syndrome.
The onset of the disease is usually between the ages of 10 and 15; however, it can occur at any age. Girls outnumber boys 8:1, but the ratio drops to 4:1 in adolescent cases. The disease is more common in people of color. It is found worldwide. Genetic factors play a role, and a family history of SLE or lupus erythematosus or an inherited complement deficiency in any form is a risk factor for developing the disease.
Childhood SLE is a chronic, noncurable disease that is treated with a variety of medications that impact immune function.
There are drug-induced forms of the disease with a differing pattern of autoimmunity and clinical profile.
Related topics: bullous systemic lupus erythematosus, discoid lupus erythematosus, oral lupus erythematosus, subacute cutaneous lupus erythematosus, tumid lupus erythematosus, lupus panniculitis
Systemic lupus erythematosus (SLE) is a disease of unclear etiology characterized by immune abnormalities and multiorgan involvement. Approximately 15%-20% of patients with SLE will present during the first 2 decades of life. Childhood-onset SLE is a phenotype of SLE that presents in childhood or adolescence. It is relatively rare, with a worldwide prevalence estimated at 1.89-25.7 per 100 000 children. On average, it presents with a more aggressive phenotype than adult-onset SLE. Constitutional symptoms, fever, fatigue, anemia, weight loss, headache, mood disturbances, arthralgias, and skin findings may all be seen. Fatigue and weight loss may be exacerbated by generalized nutritional complications associated with SLE and can sometimes be extreme. Choreiform movements may occur. Neurologic and renal involvement is a prominent characteristic in childhood SLE and often portends greater disease morbidity. Childhood SLE is also associated with chronic cardiopulmonary disease and macrophage activation syndrome.
The onset of the disease is usually between the ages of 10 and 15; however, it can occur at any age. Girls outnumber boys 8:1, but the ratio drops to 4:1 in adolescent cases. The disease is more common in people of color. It is found worldwide. Genetic factors play a role, and a family history of SLE or lupus erythematosus or an inherited complement deficiency in any form is a risk factor for developing the disease.
Childhood SLE is a chronic, noncurable disease that is treated with a variety of medications that impact immune function.
There are drug-induced forms of the disease with a differing pattern of autoimmunity and clinical profile.
Related topics: bullous systemic lupus erythematosus, discoid lupus erythematosus, oral lupus erythematosus, subacute cutaneous lupus erythematosus, tumid lupus erythematosus, lupus panniculitis
Codes
ICD10CM:
M32.9 – Systemic lupus erythematosus, unspecified
SNOMEDCT:
55464009 – Systemic lupus erythematosus
M32.9 – Systemic lupus erythematosus, unspecified
SNOMEDCT:
55464009 – Systemic lupus erythematosus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:02/07/2019
Last Updated:03/19/2024
Last Updated:03/19/2024
 Patient Information for Systemic lupus erythematosus in Child
Patient Information for Systemic lupus erythematosus in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Systemic lupus erythematosus in Child
See also in: Nail and Distal Digit