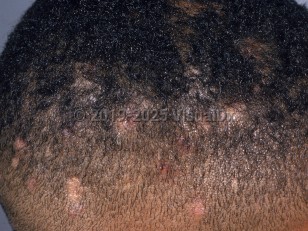
Tinea capitis in Adult
Alerts and Notices
Important News & Links
Synopsis

Tinea capitis (scalp ringworm) is a fungal infection of the scalp and hair caused by different species of dermatophytes, most often those of the genera Trichophyton and Microsporum. Most cases occur between the ages of 3 and 7 years, although tinea capitis has been reported in infants and older children, and in adults as well. It is estimated that 3%-11% of all tinea capitis cases in the world occur in adults.
Transmission is through direct contact with the infectious agents, either from affected children, animals, soil, or indirectly through fomites, including hats, hairbrushes and combs, and other instruments used in hair grooming. Some adults have tinea capitis that went untreated in childhood. Of adults, postmenopausal women are most often affected by tinea capitis.
Endothrix infections are those in which fungal spores of the dermatophyte (arthrospores) invade the hair shaft. Trichophyton tonsurans is the most common causative species, and Trichophyton violaceum may also be responsible. Black dot tinea capitis is a common presentation of endothrix infections. Patchy alopecia and broken hairs are seen. The "black dots" refer to the ends of broken-off hairs close to the scalp.
In ectothrix infections, arthrospores do not invade the hair shaft. Microsporum species, such as Microsporum canis, and other Trichophyton species, such as Trichophyton verrucosum, cause ectothrix.
Immunocompromised patient considerations: Immunosuppression (HIV, corticosteroid therapy, renal transplantation) may predispose adults to infection. Severe tinea capitis, along with Majocchi-like granulomas, deep ulcerated fungal infections, tinea corporis, and fungal nail involvement, are characteristic of an inherited deficiency of CARD9 (caspase recruitment domain-containing protein 9), an inflammatory cascade-associated protein. The disorder is autosomal recessive and is most common in North Africa countries.
Related topics: favus, kerion
Transmission is through direct contact with the infectious agents, either from affected children, animals, soil, or indirectly through fomites, including hats, hairbrushes and combs, and other instruments used in hair grooming. Some adults have tinea capitis that went untreated in childhood. Of adults, postmenopausal women are most often affected by tinea capitis.
Endothrix infections are those in which fungal spores of the dermatophyte (arthrospores) invade the hair shaft. Trichophyton tonsurans is the most common causative species, and Trichophyton violaceum may also be responsible. Black dot tinea capitis is a common presentation of endothrix infections. Patchy alopecia and broken hairs are seen. The "black dots" refer to the ends of broken-off hairs close to the scalp.
In ectothrix infections, arthrospores do not invade the hair shaft. Microsporum species, such as Microsporum canis, and other Trichophyton species, such as Trichophyton verrucosum, cause ectothrix.
Immunocompromised patient considerations: Immunosuppression (HIV, corticosteroid therapy, renal transplantation) may predispose adults to infection. Severe tinea capitis, along with Majocchi-like granulomas, deep ulcerated fungal infections, tinea corporis, and fungal nail involvement, are characteristic of an inherited deficiency of CARD9 (caspase recruitment domain-containing protein 9), an inflammatory cascade-associated protein. The disorder is autosomal recessive and is most common in North Africa countries.
Related topics: favus, kerion
Codes
ICD10CM:
B35.0 – Tinea barbae and tinea capitis
SNOMEDCT:
5441008 – Tinea capitis
B35.0 – Tinea barbae and tinea capitis
SNOMEDCT:
5441008 – Tinea capitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/18/2025
Last Updated:05/28/2025
Last Updated:05/28/2025
 Patient Information for Tinea capitis in Adult
Patient Information for Tinea capitis in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Tinea capitis in Adult