Children are most susceptible to TSS between the ages of 6 months and 2 years. Before 6 months, the birthing parent's antibodies are protective, and after age 2 years, the child begins producing antibody titers in higher amounts. TSS mortality rates are much lower in children than adults, at 5%-10% and 3%-5% for streptococcal versus staphylococcal types, respectively.
Note: An increase in invasive S pyogenes (invasive group A streptococcal [iGAS]) infections in children, including necrotizing fasciitis and streptococcal TSS, has been reported in Europe and the United States in 2022-2023.
Staphylococcal TSS is caused by S aureus strains that can produce the toxic shock syndrome toxin-1 (TSST-1). TSST-1 is believed to cause disease via direct effects on end organs, impairing clearance of gut-flora-derived endotoxins, with TSST-1 acting as a superantigen leading to massive nonspecific activation of T cells, cytokine release, and subsequent inflammation and vascular leakage. Staphylococcal TSS was identified in and most commonly affected menstruating young White females using tampons in the 1980s, but cases of menstrual TSS have declined with increased public education on tampon usage and TSS as well as the discontinuation of high-absorbency tampons. Current staphylococcal TSS cases are seen in postsurgical interventions, burn patients, patients with dialysis lines, and those with nasal packing. TSS following nasal surgery with packing is estimated to occur in approximately 16.5/100 00 of nasal surgeries performed. The prevalence in dialysis patients is unknown but thought to be rare.
Clinically, there is high fever that may be accompanied by hypotension. The dermatologic manifestations of staphylococcal TSS include the following:
- Diffuse erythematous patches that begin on the trunk and spread toward the extremities
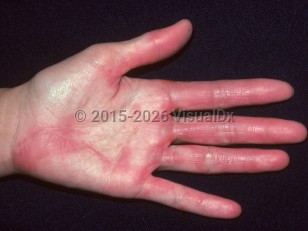
- Erythema and swelling of the palms and soles with or without generalized nonpitting edema
- Desquamation, primarily of the palms and soles, that begins 1-3 weeks after the initial onset of the rash
- Erythema of the mucous membranes (strawberry tongue and conjunctival hyperemia)
In a single-institution retrospective study of 58 pediatric patients meeting the criteria for TSS, vomiting and rash were present in most patients. However, 48% of patients with streptococcal-associated TSS had no rash. Other pertinent findings seen in this study were the presence of pulmonary infiltrates in most cases of TSS at initial diagnosis. Pyuria was also seen in approximately half of patients with streptococcal TSS. Compared to staphylococcus-induced TSS, patients with streptococcal TSS had a lower age, body mass index (BMI), and incidence of rash; however, they were more likely to have severe illness, capillary leak, pulmonary infiltrates at diagnosis, and a prolonged hospital stay.
All forms of TSS can result in end organ damage presenting as confusion and coma, renal impairment, liver impairment, adult respiratory distress syndrome, and disseminated intravascular coagulation. Supportive measures (eg, intravenous fluids, vasopressors) and appropriate antibiotics are the mainstays of treatment.
Immunocompromised patient considerations: Although infections with S aureus are common in HIV-infected individuals, the complication of TSS is rare. This is thought to be related to the immune deficits and T-helper cell dysfunction seen in HIV disease. However, in cases that have been reported, they tend to present with a recurrent and prolonged disease course. Attributed to delayed antibody production against TSST-1 by HIV-infected individuals, a protracted disease course has been reported in HIV-infected adolescents, adults, and children.