Human infection may occur from the following:
- Ingestion of oocysts in contaminated food or water
- Ingestion of tissue cysts contained in undercooked meat (particularly pork, lamb, bear, and deer) or from tissue cysts in transplanted organs (kidney and heart)
- Intake of tachyzoites (congenital infection and, rarely, from blood transfusions or laboratory accidents)
The incidence of toxoplasmosis increases with increasing age but does not vary significantly by sex. The seroprevalence of antibodies to T gondii in the United States is about 20%. Seroprevalence rates are much higher in Europe, Africa, and Central and South America.
Acute primary toxoplasmosis in the immunocompetent host most commonly causes an asymptomatic infection (80%-90%). Cervical lymphadenopathy, particularly of the posterior cervical nodes, without other associated signs or symptoms is the most common clinical manifestation. Other lymph node groups may also be involved. Enlarged nodes are usually smooth, firm, mobile, and nontender and do not suppurate. The lymphadenopathy resolves spontaneously over weeks to months. It has been estimated that up to 7% of clinically significant lymphadenopathies are caused by toxoplasmosis.
Very rarely a mononucleosis-like syndrome may occur with headache, fever, sore throat, lymphadenopathy, fatigue, myalgia, arthralgias, malaise, hepatosplenomegaly, macular erythematous rash (during the first week of illness), mild elevations in the serum transaminases, and the presence of atypical lymphocytes on the peripheral blood smear. Some patients may present with only a few of the above features. It is thought that less than 1% of mononucleosis-like syndromes are caused by acute toxoplasmosis. Very rarely, severe disseminated toxoplasmosis may occur in an apparently healthy adult. Depending on the specific organ involved, it may present as encephalitis, myocarditis, hepatitis, polymyositis, or pneumonitis.
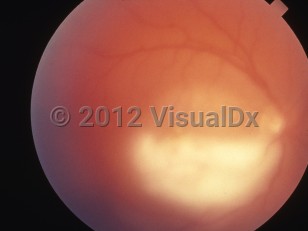
Ocular toxoplasmosis can result from congenital infection or from reactivation of latent postnatally acquired infection and rarely develops during acute infection. Toxoplasma gondii is the most common cause of chorioretinitis in immunocompetent adults. The prevalence of ocular toxoplasmosis is unknown but has been estimated at 2% of seropositive patients. Relapse, even after therapy, particularly in the eye initially involved, is the rule. Patients may complain of blurry vision, scotoma, photophobia, redness, and excessive lacrimation. Atypical findings include eye pain, prominent retinal hemorrhage, and lack of retinal scarring on ophthalmologic examination. They warrant polymerase chain reaction (PCR) testing of the vitreous or aqueous fluid for toxoplasma DNA to confirm the diagnosis. Some patients are asymptomatic.
Pregnant Patient Considerations:
Acute T gondii infection in pregnant individuals is usually asymptomatic. The most frequent clinical manifestation is regional lymphadenopathy. Acute maternal infection can result in transmission to the fetus. However, the risk of fetal transmission is not increased if maternal infection is symptomatic. With rare exceptions (infection within 3 months of conception or maternal immunosuppressed state), women previously infected with T gondii, and therefore seropositive for anti-toxoplasma antibodies prior to pregnancy, are protected from transmitting the infection to their fetuses. HIV-infected women with latent toxoplasmosis may have reactivation of latent infection, which can result in fetal transmission. The incidence of fetal transmission is highest during second- and third-trimester maternal infection. Although less frequent, fetal transmission during first-trimester maternal infection more commonly results in severe illness in the newborn. See congenital toxoplasmosis.
Immunocompromised Patient Considerations:
Seronegative organ transplant recipients from a T gondii-seropositive donor, seropositive hematopoietic stem cell transplant recipients, patients with AIDS, and those receiving corticosteroids are at risk for disease caused by reactivation of chronic latent T gondii infection. Primary toxoplasmosis is very rare but can cause disseminated disease, which is frequently fatal. The most common presentation of reactivation of latent infection is toxoplasmic encephalitis and much less frequently chorioretinitis; other organ involvement (pneumonitis, myocarditis) occurs rarely. Manifestations of toxoplasmic encephalitis include focal neurological deficits (hemiparesis, speech abnormalities, altered mental status, movement disorders), seizures, headache, and fever.