The initial infection is frequently acquired before 2 years of age, and recurrent infection causes chronic inflammation with scarring of the cornea, which can lead to blindness if untreated. Worldwide, trachoma is the most preventable cause of infectious blindness.
Clinical manifestations of trachoma can be divided into 2 clinical phases: active trachoma and cicatricial disease.
Active trachoma – Active trachoma is mostly seen in young children and occurs after a 5-10 day incubation period from exposure. While most individuals are asymptomatic, signs and symptoms can include the following:
- Swelling of the eyelids from formation of follicles on the superior tarsal conjunctiva
- Eye irritation
- Mucopurulent discharge
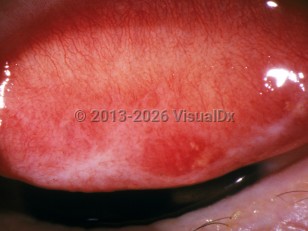
- Marked conjunctival inflammation
- Entropion – Conjunctival scarring leading to inward turning of the eyelid
- Trichiasis – Ingrown eyelashes from entropion causing irritation of eyeball and cornea
- Corneal edema, ulceration, and scarring due to trichiasis, resulting in corneal pannus (inflammatory vascular tissue) followed by corneal opacity, and eventually blindness