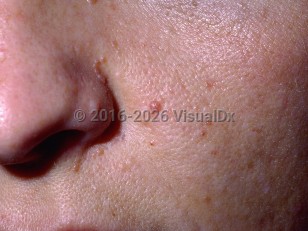
Tuberous sclerosis in Infant/Neonate
Alerts and Notices
Important News & Links
Synopsis

Tuberous sclerosis (TS), or tuberous sclerosis complex (TSC), also known as Bourneville disease, is an autosomal dominant, multisystem disorder caused by mutations in the genes for the proteins hamartin and tuberin. It is characterized by tumor-like growths, or hamartomas, in almost every organ. Two-thirds of infants with TS/TSC are born to unaffected parents as a result of a sporadic mutation. During the neonate period and infancy, the most common presenting signs are seizures or cardiac rhabdomyomas, typically found on routine antenatal screening.
A majority of TSC patients will have epilepsy, and more than half will have developmental delays collectively termed TSC-associated neuropsychiatric disorders (TAND). Brain lesions including glioneuronal hamartomas and periventricular giant cell astrocytomas are commonly identified in patients with TAND.
Establishing the diagnosis of TS can be challenging due to the wide variation in severity and age-related penetrance of clinical manifestations. In some cases, diagnosis may be delayed until adolescence or adulthood.
A majority of TSC patients will have epilepsy, and more than half will have developmental delays collectively termed TSC-associated neuropsychiatric disorders (TAND). Brain lesions including glioneuronal hamartomas and periventricular giant cell astrocytomas are commonly identified in patients with TAND.
Establishing the diagnosis of TS can be challenging due to the wide variation in severity and age-related penetrance of clinical manifestations. In some cases, diagnosis may be delayed until adolescence or adulthood.
Codes
ICD10CM:
Q85.1 – Tuberous sclerosis
SNOMEDCT:
7199000 – Tuberous sclerosis
Q85.1 – Tuberous sclerosis
SNOMEDCT:
7199000 – Tuberous sclerosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/07/2018
Last Updated:01/25/2022
Last Updated:01/25/2022
Tuberous sclerosis in Infant/Neonate