Ulcerative colitis in Adult
Alerts and Notices
Important News & Links
Synopsis
The pathophysiology has not been fully elucidated. There are hypothesized genetic, environmental, and immune factors that likely contribute to the development of UC. Most likely, the etiology is multifactorial.
Clinical manifestations include relapsing episodes of bloody diarrhea, abdominal pain, fever, malaise, and weight loss. Patients may be anemic.
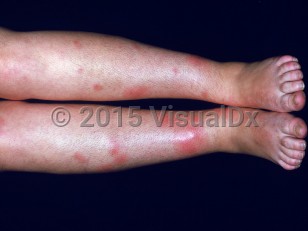
UC is associated with extraintestinal manifestations. These include dermatologic conditions (ie, erythema nodosum, pyoderma gangrenosum, psoriasis), inflammatory arthritis, uveitis, and primary sclerosing cholangitis.
Although 83% of patients will suffer from at least one relapse during the first 10 years after initial onset, the prognosis for UC in general is good. Over half of patients report remission or only mild intestinal symptoms.
On endoscopy, UC almost always presents with continuous involvement of the rectum and/or colon. During the active phase of disease, the mucosa can appear erythematous and friable. Pseudopolyps and inflammatory polyps may also be present as a result of chronic inflammation.
Risk factors: UC is most common in developed countries. This is suggestive of environmental risk factors for the development of UC.
There are myriad genes associated with UC, but no identifiable genetic cause of UC.
Smoking cessation is a risk factor for the development of UC.
Timeline: The course of UC is unpredictable. The initial presentation can vary from mild / asymptomatic to severe (toxic hemorrhagic colitis). Some patients have a quiescent disease course, while others can have progressive worsening of bowel inflammation.
Pediatric patient considerations: The mean age at time of diagnosis of IBD among children is 10.3 years. Pediatric-onset disease has a worse course, with more extensive disease, a higher colectomy rate (30%-40% at 10 years compared with 20% in adult-onset disease), and more frequent hospitalizations.
Codes
K51.90 – Ulcerative colitis, unspecified, without complications
SNOMEDCT:
64766004 – Ulcerative colitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/12/2024