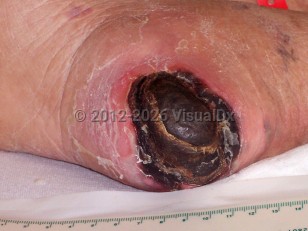
A pressure injury results from local injury to the skin or deeper tissue, usually over a bony prominence. The injury is caused by pressure or other factors, such as shear or friction, with moisture playing a major contributory role.
Other risk factors that predispose to ulcer formation are prolonged immobility, malnutrition, fecal/urinary incontinence, altered mental status, dry skin, and chronic systemic conditions. The most common location of pressure injury is the sacrum, followed by the heels. The age group most likely to develop pressure injuries is the elderly. This can be either in the setting of the hospital, where it is commonly seen following hip surgery, or in nursing homes or assisted-living facilities.
In unstageable pressure injuries, accurate documentation is difficult because depth is not visible. The following criteria should be assessed, where possible:
- Size of the ulcer, including width and length in centimeters
- Presence of eschar tissue
- Presence of necrotic tissue
- Drainage; exudate – If present, the color and amount.
- Wound edges – Look carefully at the edge of the ulcer for evidence of induration, maceration, rolling edges, and redness.
- Skin around the edges of the ulcer – Periwound skin should be assessed for color, texture, temperature, and integrity of the surrounding skin.
- Presence of undermining, tunneling, and sinus tracts. Tunneling is a passage that extends from the wound through to subcutaneous tissue or muscle. Undermining is the destruction of tissue around the edge of that wound.
- Presence or absence of pain
- Odor, if present or absent
- Medical device-related pressure injury (describes an etiology) – Results from the use of devices designed and applied for therapeutic purposes. Injury generally conforms to the pattern or shape of the device. Stage using the staging system.
- Mucosal membrane pressure injury – Found on mucous membranes with a history of a medical device in use at the location of the injury. Cannot be staged due to anatomy of tissue.