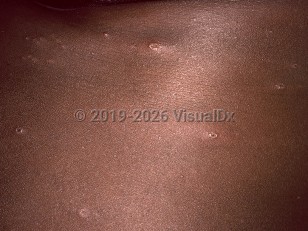
Varicella in Adult
Alerts and Notices
Important News & Links
Synopsis

Varicella, also known as chickenpox, is a self-limited viral infection caused by varicella-zoster virus (VZV), a member of the Herpesviridae family. Prior to the clinical implementation of the varicella vaccine, more than 99% of adults aged 40 and older had evidence of previous infection. Transmission occurs via airborne respiratory droplets or direct contact with vesicular fluid. The incubation period ranges from 10-20 days.
VZV is an acute, serious viral infection when it occurs in adults. In adults, a 2- to 3-day prodrome of fever, chills, irritability, headache, and myalgias may occur. However, skin lesions are usually the initial manifestation of the disease: an acute eruption of pruritic, erythematous macules and papules that start on the face, oral mucosa, and scalp and spread to the trunk and extremities. The lesions rapidly evolve into 1- to 3-mm vesicles with clear serous fluid on an erythematous background. The hallmark of chickenpox is the presence of lesions in various stages of development. Older lesions will evolve to form pustules and serous crusts that heal within 10 days of time. Fever is variable, usually less than 38.9°C (102°F), but can be anywhere from normal to 40.6°C (105°F) in severe cases.
The most common complication is secondary infection of lesions with Staphylococcus or beta-hemolytic Streptococcus. The streptococcal infection can progress to necrotizing fasciitis. Varicella pneumonia is more common in adults, can lead to adult respiratory distress syndrome, and has an overall mortality rate between 10% and 30%. According to the US Centers for Disease Control and Prevention (CDC), adults have a 25-fold greater mortality risk compared with children aged 1-4.
Less common complications include purpura fulminans and thrombocytopenia with protein S deficiency, orchitis, hepatitis, uveitis, arthritis, myocarditis, nephritis, macular atrophy, gastrointestinal bleeding, bacterial pneumonia, protein-losing enteropathy, intracranial vasculopathy, and Reye syndrome. Central nervous system (CNS) complications occur rarely. These include aseptic meningitis, dystonia, myelitis, cerebellar ataxia, Guillain-Barré, and encephalitis. The cerebellar form of encephalitis has a high mortality rate in adults.
One varicella episode usually confers lifelong immunity, although reinfections have been documented.
In vaccinated individuals, "breakthrough varicella" can occur. Illness is usually mild (low fever or no fever, fewer lesions [less than 50], less pruritic, shorter duration, absence of vesicles), although some patients present similar to unvaccinated individuals.
Patients are considered contagious for 2-5 days before the onset of cutaneous lesions and for 6 days after the last crop has appeared.
Prior to the clinical implementation of the varicella vaccine, approximately 100 deaths per year in the United States were attributed to acute varicella. The highest incidence is from March to May.
Immunocompromised Patient Considerations
Pregnant patients may be at increased risk for severe illness from varicella. Maternal varicella in the first 20 weeks of pregnancy is associated with a 2% risk of fetal damage. If maternal varicella occurs near the time of delivery, the neonate is at risk for severe neonatal varicella.
Varicella may be severe in human immunodeficiency virus (HIV)-infected and other immunocompromised individuals (particularly those with lymphoma and those receiving immunosuppressive therapy, including systemic steroid therapy), with a 7%-10% mortality rate. These patients often have a more extensive (disseminated) and atypical eruption (often with purpura and hemorrhagic vesicles) as well as visceral involvement (CNS, lung, liver). HIV-infected patients have a 7-15 times greater risk of developing herpes zoster.
VZV is an acute, serious viral infection when it occurs in adults. In adults, a 2- to 3-day prodrome of fever, chills, irritability, headache, and myalgias may occur. However, skin lesions are usually the initial manifestation of the disease: an acute eruption of pruritic, erythematous macules and papules that start on the face, oral mucosa, and scalp and spread to the trunk and extremities. The lesions rapidly evolve into 1- to 3-mm vesicles with clear serous fluid on an erythematous background. The hallmark of chickenpox is the presence of lesions in various stages of development. Older lesions will evolve to form pustules and serous crusts that heal within 10 days of time. Fever is variable, usually less than 38.9°C (102°F), but can be anywhere from normal to 40.6°C (105°F) in severe cases.
The most common complication is secondary infection of lesions with Staphylococcus or beta-hemolytic Streptococcus. The streptococcal infection can progress to necrotizing fasciitis. Varicella pneumonia is more common in adults, can lead to adult respiratory distress syndrome, and has an overall mortality rate between 10% and 30%. According to the US Centers for Disease Control and Prevention (CDC), adults have a 25-fold greater mortality risk compared with children aged 1-4.
Less common complications include purpura fulminans and thrombocytopenia with protein S deficiency, orchitis, hepatitis, uveitis, arthritis, myocarditis, nephritis, macular atrophy, gastrointestinal bleeding, bacterial pneumonia, protein-losing enteropathy, intracranial vasculopathy, and Reye syndrome. Central nervous system (CNS) complications occur rarely. These include aseptic meningitis, dystonia, myelitis, cerebellar ataxia, Guillain-Barré, and encephalitis. The cerebellar form of encephalitis has a high mortality rate in adults.
One varicella episode usually confers lifelong immunity, although reinfections have been documented.
In vaccinated individuals, "breakthrough varicella" can occur. Illness is usually mild (low fever or no fever, fewer lesions [less than 50], less pruritic, shorter duration, absence of vesicles), although some patients present similar to unvaccinated individuals.
Patients are considered contagious for 2-5 days before the onset of cutaneous lesions and for 6 days after the last crop has appeared.
Prior to the clinical implementation of the varicella vaccine, approximately 100 deaths per year in the United States were attributed to acute varicella. The highest incidence is from March to May.
Immunocompromised Patient Considerations
Pregnant patients may be at increased risk for severe illness from varicella. Maternal varicella in the first 20 weeks of pregnancy is associated with a 2% risk of fetal damage. If maternal varicella occurs near the time of delivery, the neonate is at risk for severe neonatal varicella.
Varicella may be severe in human immunodeficiency virus (HIV)-infected and other immunocompromised individuals (particularly those with lymphoma and those receiving immunosuppressive therapy, including systemic steroid therapy), with a 7%-10% mortality rate. These patients often have a more extensive (disseminated) and atypical eruption (often with purpura and hemorrhagic vesicles) as well as visceral involvement (CNS, lung, liver). HIV-infected patients have a 7-15 times greater risk of developing herpes zoster.
Codes
ICD10CM:
B01.9 – Varicella without complication
SNOMEDCT:
38907003 – Varicella
B01.9 – Varicella without complication
SNOMEDCT:
38907003 – Varicella
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:05/06/2025
 Patient Information for Varicella in Adult
Patient Information for Varicella in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Varicella in Adult