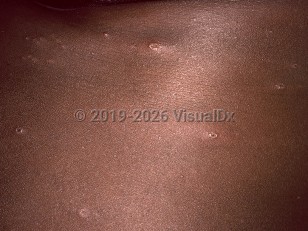
Varicella in Child
Alerts and Notices
Important News & Links
Synopsis

This summary discusses varicella in children. Neonatal varicella is addressed separately.
Varicella, or chickenpox, is an acute, highly contagious exanthem caused by primary infection with varicella-zoster virus (VZV). The virus is believed to be spread by respiratory droplets, including airborne, and skin vesicles from individuals with varicella or herpes zoster (a dermatomal rash caused by reactivated endogenous VZV) to the respiratory tract of susceptible children. In immunologically normal children, the illness typically begins after an incubation period of 2-3 weeks, lasts 3-7 days, and resolves without complication. One varicella episode usually confers lifelong immunity, although reinfections have been documented.
In rare cases, varicella is associated with prolonged courses and severe complications, including bacterial superinfection, pneumonia, encephalitis, bleeding disorders, and hepatitis. Adolescents and immunocompromised children (eg, those with malignancy, congenital defects in cell-mediated immunity, or organ transplant; children receiving long-term immunosuppressive therapy; and HIV-infected children) are at elevated risk for complications.
Varicella was a common viral disease of children in the United States until childhood vaccination became routine during the 1990s. The disease remains common in underdeveloped countries and is seen more frequently in older children and adults.
In vaccinated individuals, "breakthrough varicella" can occur. Illness is usually mild (low fever or no fever, fewer lesions [less than 50], less pruritic, shorter duration, absence of vesicles), although some patients present similar to unvaccinated individuals.
Note: Pediatric invasive group A streptococcal (iGAS) infections and noninvasive group A streptococcal infection cases have been associated with respiratory infections due to viruses including parainfluenza, rhinovirus, enterovirus, influenza, and human metapneumovirus. Concurrent or preceding viral infections, including varicella, may increase risk for iGAS infection. Severe outcomes include necrotizing fasciitis, streptococcal toxic shock syndrome, and death.
Related topic: varicella pneumonia
Varicella, or chickenpox, is an acute, highly contagious exanthem caused by primary infection with varicella-zoster virus (VZV). The virus is believed to be spread by respiratory droplets, including airborne, and skin vesicles from individuals with varicella or herpes zoster (a dermatomal rash caused by reactivated endogenous VZV) to the respiratory tract of susceptible children. In immunologically normal children, the illness typically begins after an incubation period of 2-3 weeks, lasts 3-7 days, and resolves without complication. One varicella episode usually confers lifelong immunity, although reinfections have been documented.
In rare cases, varicella is associated with prolonged courses and severe complications, including bacterial superinfection, pneumonia, encephalitis, bleeding disorders, and hepatitis. Adolescents and immunocompromised children (eg, those with malignancy, congenital defects in cell-mediated immunity, or organ transplant; children receiving long-term immunosuppressive therapy; and HIV-infected children) are at elevated risk for complications.
Varicella was a common viral disease of children in the United States until childhood vaccination became routine during the 1990s. The disease remains common in underdeveloped countries and is seen more frequently in older children and adults.
In vaccinated individuals, "breakthrough varicella" can occur. Illness is usually mild (low fever or no fever, fewer lesions [less than 50], less pruritic, shorter duration, absence of vesicles), although some patients present similar to unvaccinated individuals.
Note: Pediatric invasive group A streptococcal (iGAS) infections and noninvasive group A streptococcal infection cases have been associated with respiratory infections due to viruses including parainfluenza, rhinovirus, enterovirus, influenza, and human metapneumovirus. Concurrent or preceding viral infections, including varicella, may increase risk for iGAS infection. Severe outcomes include necrotizing fasciitis, streptococcal toxic shock syndrome, and death.
Related topic: varicella pneumonia
Codes
ICD10CM:
B01.9 – Varicella without complication
SNOMEDCT:
38907003 – Varicella
B01.9 – Varicella without complication
SNOMEDCT:
38907003 – Varicella
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/12/2025
Last Updated:05/13/2025
Last Updated:05/13/2025
 Patient Information for Varicella in Child
Patient Information for Varicella in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Varicella in Child