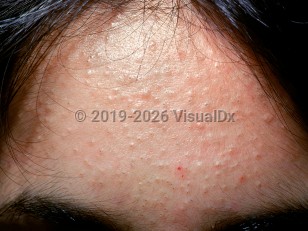
Acne vulgaris in Child
Alerts and Notices
Important News & Links
Synopsis

Acne vulgaris is an extremely common, usually self-limited, chronic inflammatory condition of the pilosebaceous unit. The pathogenesis involves multiple factors, including (1) increased sebum production, (2) follicular hyperkeratinization and corneocyte hypercohesiveness, (3) proliferation of the bacterium Cutibacterium acnes (formerly known as Propionibacterium acnes), and (4) inflammation that is neutrophil driven in early lesions and Th1/Th17 driven in established lesions. Acne vulgaris typically begins at puberty as a result of androgen stimulation of the pilosebaceous unit and changes in the keratinization at the follicular orifice.
There is a wide spectrum of clinical disease, ranging from a few comedones to many inflamed papules, pustules, and nodules. While there is no single severity grading system that has been adopted by all clinicians, the Investigator Global Assessment (IGA) is most commonly utilized in the United States.
Acne vulgaris is most commonly diagnosed among the adolescent patient population. It is most commonly found on areas of skin with the greatest density of sebaceous follicles, such as the face, back, and upper chest. Acne can affect people of every race and ethnicity. Acne can last through the teenage years into adulthood.
Some studies report that acne vulgaris is slightly more common in adolescent females than in their adolescent male counterparts. Patients with endocrinopathies producing hyperandrogenic states (ie, HAIR-AN syndrome [hyperandrogenism, insulin resistance, and acanthosis nigricans], polycystic ovary syndrome [PCOS]) and hypercorticism (ie, Cushing syndrome, ectopic ACTH syndrome, congenital adrenal hyperplasia) also present with an increased risk of developing acne. While a benign condition, acne can lead to permanent scarring and disfigurement and has been associated with significant psychosocial distress, such as anxiety and depression. Therefore, initiation of treatment in the earliest stages is preferable. Infantile acne is associated with a higher risk of developing severe acne during adolescence.
Certain drugs can exacerbate acne vulgaris, such as medroxyprogesterone, low-estrogen oral contraceptives, the progesterone-only birth control pill, JAK inhibitors, and exacaftor / tezacaftor / ivacaftor, used in the treatment of cystic fibrosis. Medications can also induce acneiform eruptions. See drug-induced acneiform eruptions for additional information.
Related topics: acne conglobata, acne excoriée, acne fulminans, acne mechanica, acne necrotica, cosmetic-induced acne
Codes
L70.0 – Acne vulgaris
SNOMEDCT:
88616000 – Acne vulgaris
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:10/30/2025
 Patient Information for Acne vulgaris in Child
Patient Information for Acne vulgaris in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient