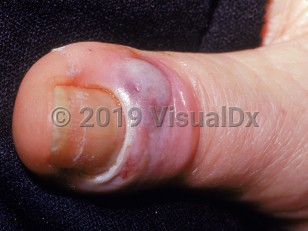
Acute paronychia frequently arises from trauma to one of the nail folds, resulting in compromise of the physiologic barrier to entry of microorganisms. Inflammation may proceed to bacterial infection, resulting in pus. In some cases, the abscess tracks under the nail plate, and if not treated quickly, it can result in permanent damage to the nail matrix.
Examples of inciting trauma include foreign bodies, such as splinters; manipulations, such as manicures or pedicures; ingrown nails; fingernail biting; finger sucking in children; or "hangnail" removal. Occasionally, acute paronychia arises as a painful exacerbation of chronic paronychia, which is now understood to be a localized form of chronic irritant or allergic dermatitis.
Certain drugs – including retinoids (isotretinoin, acitretin), methotrexate, antiretroviral protease inhibitors (indinavir, lamivudine), and epidermal growth factor receptor (EGF) inhibitors (cetuximab, gefitinib, lapatinib) – can cause drug-induced paronychia, in some cases with associated periungual lobular capillary hemangioma (pyogenic granuloma).
Specific bacteria predominate in trauma-related acute paronychia. They include Staphylococcus aureus, Streptococcus pyogenes, and anaerobic bacteria derived from the oral flora. Mixed bacterial flora are common. Other bacteria that have been reported as causes include:
- Pseudomonas
- Enterococcus faecalis
- Enterobacter cloacae
- Proteus
- Hendersonula
- Scytalidium
- Fusarium
- Prevotella
- Bartonella



 Patient Information for
Patient Information for