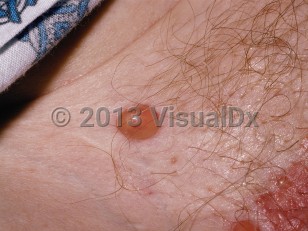
Bullous pemphigoid
Alerts and Notices
Important News & Links
Synopsis

Bullous pemphigoid (BP) is an autoimmune subepidermal blistering disease with average onset at around 60 years of age. There is no ethnic or sex predilection.
Pathogenesis includes development of autoantibodies against hemidesmosome adhesion complex in the basement membrane of the skin (BP180 and/or BP230), resulting in complement activation, mast cell degranulation, release of inflammatory mediators, and recruitment of neutrophils and eosinophils. This leads to the formation of localized or generalized urticarial plaques, erythematous papules or plaques, and/or bullae. The disease can occur on any body surface, but mucous membrane involvement is seen in only 10%-30% of patients.
BP has variable clinical presentation as well as disease course. Presentation can range from itch without rash to localized or generalized eruptions. The morphology may be variable: some presentations are nonbullous, in which case urticarial or eczematous-appearing papules and plaques, or excoriations only, may be seen. The localized variant can mimic dyshidrosis when on the palms or soles and can develop in sites of radiation, surgery, prior photodynamic therapy, infection, paralysis, and venous stasis, as well as adjacent to ostomies. Disease course ranges from self-limiting to chronic over months to years.
Peripheral eosinophilia can be seen in approximately 50% of patients and is positively correlated with disease severity. Its presence has also been correlated with older age and palmoplantar involvement. Lack of peripheral eosinophilia has been positively correlated with younger age and mucosal disease.
BP is associated with neurologic disease ranging from stroke to dementia. Relapse of BP has been shown to be more likely in individuals with extensive disease and dementia. BP is also been associated with other autoimmune diseases such as diabetes mellitus, thyroiditis, dermatomyositis, systemic lupus erythematosus, rheumatoid arthritis, ulcerative colitis, myasthenia gravis, and multiple sclerosis in case reports and case series. A population-based study from Finland strongly suggests an increased risk of BP in patients with dermatitis herpetiformis. Medications (ie, furosemide, NSAIDs, captopril, penicillamine, gliptins, PD-1 and PDL-1 inhibitors, and some antibiotics) have also been associated with triggering BP.
Codes
L12.0 – Bullous pemphigoid
SNOMEDCT:
77090002 – Bullous pemphigoid
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/04/2023