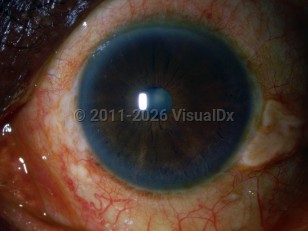
Cataracts - External and Internal Eye
Alerts and Notices
Important News & Links
Synopsis

Though cataract formation is a naturally occurring event, several medical conditions can predispose or accelerate formation. Patients with diabetes, hypocalcemia (hypoparathyroid), myotonic dystrophy, high myopia, and inherited metabolic conditions may form cataracts earlier in life. Ocular trauma can also rapidly induce cataract formation.
Related topic: Congenital cataract
Codes
H26.9 – Unspecified cataract
SNOMEDCT:
193570009 – Cataract
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
 Patient Information for Cataracts - External and Internal Eye
Patient Information for Cataracts - External and Internal Eye- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient