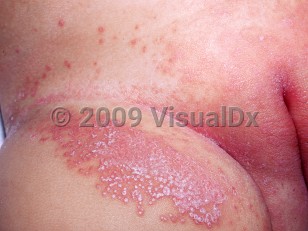
Candidal diaper dermatitis develops when sufficient moisture in the diaper area allows Candida albicans, normal flora in the mouth and gastrointestinal tract, to proliferate and invade the stratum corneum. The dermatitis usually begins around 6 weeks of age and is often associated with recent antibiotic use or diarrhea, although it can be seen without any inciting factor. It can occur in conjunction with oral thrush. Candida may also secondarily infect and exacerbate irritant diaper dermatitis, seborrheic dermatitis, and flexural psoriasis.
An alkaline pH in the diaper area predisposes a patient to candidal diaper dermatitis. In both children and adults, fecal bacteria further alkalize urinary pH, which increases the risk of candidal infections. Breast-fed infants have a lower incidence of diaper dermatitis than formula-fed infants, which is theorized to be secondary to a lower stool pH in the breast-fed infants. Furthermore, patients with a defective Th17 response are predisposed to recurrent cutaneous candidal infections.
In adults, risk factors for candidal diaper dermatitis include urinary and fecal incontinence, diabetes mellitus, obesity, human immunodeficiency virus (HIV) infection, antibiotic use, systemic immunosuppressive medications including corticosteroids, prolonged hospitalizations, nursing home stays, and bedbound patients.
Related topics: Male genital candidiasis, Vulvovaginal candidiasis
Diaper dermatitis candidiasis in Child
See also in: AnogenitalAlerts and Notices
Important News & Links
Synopsis

Codes
ICD10CM:
L22 – Diaper dermatitis
SNOMEDCT:
240711004 – Diaper candidiasis
L22 – Diaper dermatitis
SNOMEDCT:
240711004 – Diaper candidiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:12/26/2018
Last Updated:03/03/2024
Last Updated:03/03/2024
 Patient Information for Diaper dermatitis candidiasis in Child
Patient Information for Diaper dermatitis candidiasis in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today