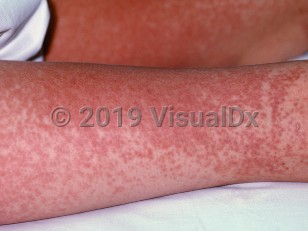
Drug-induced hypersensitivity syndrome in Child
Alerts and Notices
Important News & Links
Synopsis

Clinically, symptoms develop 2-8 weeks after initiation of the responsible drug. If a patient is rechallenged with the drug, the reaction will occur within 24 hours. Siblings of patients with DIHS have an approximately 25% chance of a similar reaction to a culprit medication. An exanthematous eruption is present in over 80% of cases and can worsen even after the withdrawal of the offending drug. Eosinophilia and/or a mononucleosis-like atypical lymphocytosis is commonly observed. The liver is the most commonly and severely affected visceral site. Myocarditis, interstitial pneumonitis, interstitial nephritis, encephalitis, myositis, pancreatitis, and thyroiditis have all been observed. Cutaneous and visceral involvement may persist for several months after discontinuation of the offending drug. The cutaneous lesions of DIHS will desquamate and often leave areas of hyper- and/or hypopigmentation that may persist for several months to 1-2 years. Some patients may experience multiple episodes of remission and relapse.
Hypothyroidism and other autoimmune conditions such as pancreatitis, myocarditis, or type 1 diabetes may develop several months after the acute phase of the illness. Vitiligo and type III polyglandular autoimmune syndrome have also been reported after DIHS / DRESS in children.
The most common drugs causing this syndrome are anticonvulsants such as phenytoin, carbamazepine, phenobarbital, and lamotrigine. DIHS secondary to anticonvulsants is occasionally referred to as anticonvulsant hypersensitivity syndrome. Sulfonamide antibiotics, allopurinol, metronidazole, and abacavir are also common causes. Any new drug taken in the preceding 2 months is considered suspect. The incidence of DIHS has been estimated to be between 1 in 1000 to 1 in 10 000 exposures to drugs such as sulfonamides and anticonvulsants.
Special considerations in neonates: DIHS / DRESS is exceedingly rare in the neonatal period. Anticonvulsants are the most commonly implicated drugs. Clinical and laboratory findings are similar to those seen in the pediatric and adult populations.
Codes
D72.12 – Drug rash with eosinophilia and systemic symptoms syndrome
SNOMEDCT:
702809001 – Drug-induced hypersensitivity syndrome
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/22/2023