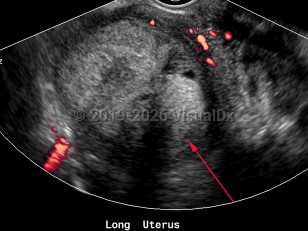
Endometrial carcinoma
Alerts and Notices
Important News & Links
Synopsis

Endometrial carcinomas are more common in White women and more likely to develop after menopause. The highest incidence worldwide is seen in the United States.
Most commonly, endometrial carcinoma develops in conditions that expose the uterus to estrogen, either for very prolonged periods of time, without opposing progesterone, or both. As such, obesity, polycystic ovarian syndrome (PCOS), diabetes mellitus type 1 and type 2, anovulation, nulliparity, tamoxifen use (in postmenopausal women), prolonged hormone replacement therapy with estrogen alone, and early menarche or late menopause are all variably potent risk factors for endometrial carcinoma.
There are genetic syndromes that predispose women to endometrial carcinoma, particularly Lynch syndrome (hereditary nonpolyposis colorectal cancer). This autosomal dominant syndrome should be strongly considered in women diagnosed with endometrial carcinoma before age 50. Lynch syndrome should also be suspected when the patient has a family history of endometrial, colorectal, ovarian, intestinal, or renal cancers. Women with Cowden syndrome also have an increased risk of endometrial cancer.
Related topic: uterine cancer
Codes
C55 – Malignant neoplasm of uterus, part unspecified
SNOMEDCT:
254878006 – Endometrial Carcinoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:04/05/2026