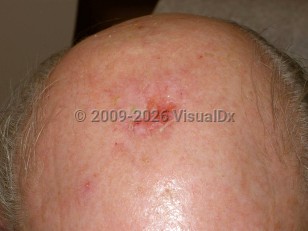
Erosive pustular dermatosis
See also in: Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

The etiology of EPD remains unknown. However, it is claimed that the major predisposing condition is cutaneous atrophy, which is primarily the result of actinic damage on the scalp and stretching of the skin secondary to the edema of venous insufficiency on the legs. EPD then develops from one or more triggering factors, eg, physical, medical, or surgical trauma. Treatment of actinic keratosis on the scalp (including liquid nitrogen and topical chemotherapeutic agents), surgical procedures (such as neurosurgery, skin grafting, hair transplant, laser therapy, and radiation therapy), physical injury, and sunburn have all been reported as provoking factors in the development of EPD of the scalp. Similarly, compression therapy has been found to be an inciting factor for EPD of the legs.
EPD is clinically characterized by sterile pustules and chronic crusted erosions. Crusts resolve leaving atrophy and scarring alopecia, and new areas of pustulation develop within a few days. Often, the presence of crusted erosions or ulcers predominates, and pustules are not seen. Itch or mild to moderate pain may be noted.
EPD has rarely been seen in patients with autoimmune disorders such as rheumatoid arthritis, Hashimoto thyroiditis, autoimmune hepatitis, and Takayasu arteritis. The significance of this is unclear.
EPD has a chronic, recurring, and slow but progressive course. Scarring alopecia and cutaneous malignancies such as basal cell carcinoma and squamous cell carcinoma may eventuate in the scar tissue.
Codes
L98.8 – Other specified disorders of the skin and subcutaneous tissue
SNOMEDCT:
403530003 – Erosive pustular dermatosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/21/2021