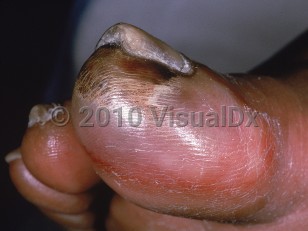
Frostbite in Adult
Alerts and Notices
Important News & Links
Synopsis

Frostnip is the earliest sign of cold injury and presents with pain and pallor of the affected area, followed by numbness. With continued exposure, complete anesthesia will result. Many experts classify frostbite injuries as either superficial or deep, as this corresponds with a functional outcome. If a thumbprint may be left in the skin, the condition is more superficial, while deeper frostbite presents with skin that is hard to the touch. In deeper cases, deeper structures such as muscle, nerve, and bone may be affected.
The severity of tissue injury correlates with duration of exposure and lowest temperature. Pain and pruritus associated with frostbite can last as long as 8 weeks and 6 months, respectively. An increased sensitivity to cold may remain in areas of prior frostbite, and arthritis of acral joints may occur.
Predisposing factors for the development of frostbite include vascular conditions (such as peripheral vascular disease), diabetes, and the use of beta blockers. Additionally, peripheral neuropathy and Raynaud phenomenon, prolonged exposure to cold or high winds, restrictive clothing, and alcohol use predispose to frostbite. Prior damage from cold also increases the risk of frostbite. Athletes training at high altitude are at increased risk because of the combination of cold exposure and low ambient oxygen tension, which makes oxygen deprivation of affected tissues more severe.
Pediatric patient considerations: Children are at increased risk for frostbite because of their increased surface to body mass ratio. Younger children may not communicate symptoms at onset.
Codes
T33.90XA – Superficial frostbite of unspecified sites, initial encounter
SNOMEDCT:
370977006 – Frostbite
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:05/09/2022
 Patient Information for Frostbite in Adult
Patient Information for Frostbite in Adult- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient