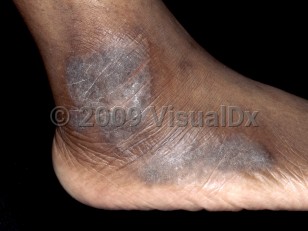
Lichen simplex chronicus in Adult
See also in: AnogenitalAlerts and Notices
Important News & Links
Synopsis

Lichen simplex chronicus (LSC) is a lichenified well-demarcated scaly plaque that is induced by chronic rubbing and/or scratching. Lichenification refers to thickened skin with enhanced skin markings that occurs as a result of friction from excessive scratching and rubbing. Co-existing papules may also be observed (prurigo nodularis), as may excoriations, which can become secondarily infected. As these plaques are self-induced, LSC is almost always found on areas that are within hand's reach, most commonly on the back of the head and neck in women and in the genital (scrotum and perineum) area in men. The lower aspect of the lateral shin is another site that is frequently involved. LSC is more common in women and middle-aged to elderly patients.
Itch from a variety of causes induces individuals to chronically scratch or rub their skin. LSC is commonly observed in uncontrolled atopic dermatitis and other forms of eczema, and in other dermatoses that have pruritus as a feature (eg, insect bites, scabies). When LSC is observed on relatively normal skin with no obvious underlying cutaneous (or systemic) precipitants, psychological factors are thought to play a significant role. In either case, an itch-scratch cycle is initiated, and if allowed to continue unabated, plaques of LSC inevitably develop.
Itch from a variety of causes induces individuals to chronically scratch or rub their skin. LSC is commonly observed in uncontrolled atopic dermatitis and other forms of eczema, and in other dermatoses that have pruritus as a feature (eg, insect bites, scabies). When LSC is observed on relatively normal skin with no obvious underlying cutaneous (or systemic) precipitants, psychological factors are thought to play a significant role. In either case, an itch-scratch cycle is initiated, and if allowed to continue unabated, plaques of LSC inevitably develop.
Codes
ICD10CM:
L28.0 – Lichen simplex chronicus
SNOMEDCT:
53891004 – Lichen simplex chronicus
L28.0 – Lichen simplex chronicus
SNOMEDCT:
53891004 – Lichen simplex chronicus
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:06/15/2016
 Patient Information for Lichen simplex chronicus in Adult
Patient Information for Lichen simplex chronicus in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Lichen simplex chronicus in Adult
See also in: Anogenital