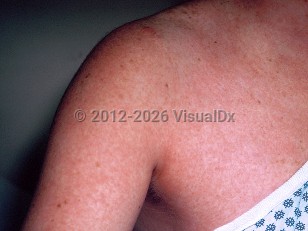
Measles in Adult
Alerts and Notices
Important News & Links
Synopsis

Measles (rubeola) is a highly contagious, infectious disease caused by a single-stranded RNA virus within the Paramyxoviridae family. The disease is worldwide in distribution. The infection primarily occurs in late winter and spring when individuals are in close contact. Cases are more common in developing countries, as the majority of individuals in industrialized nations have been vaccinated. Classically, the disease is more often seen in children. In an unvaccinated population, children younger than 5 years are at highest risk of infection and death. The disease runs a more severe course in malnourished children.
Measles is transmitted via respiratory droplets and can remain viable and transmissible for up to 2 hours in an airspace after an infected person leaves an area. The incubation period after the measles virus enters the upper respiratory mucosa is about 10 days (range 7-21 days), with the rash typically appearing about 14 days after an exposure. Infected individuals are considered contagious from about 4 days prior to the appearance of the rash through about 4 days after its appearance.
A prodrome characterized by fever (up to 40.5°C [105°F]), coryza (nasal congestion), cough, and conjunctivitis occurs for about 3-4 days followed by the onset of the rash (sometimes immunocompromised individuals do not develop the rash or develop a rash with severe desquamation). The coryza, a "barking" cough, and conjunctivitis will increase in severity until the rash reaches its peak. The US Centers for Disease Control and Prevention (CDC) reports that approximately 1 in 10 children with measles will develop otitis media, and up to 1 in 20 will develop pneumonia. Encephalitis is a complication in about 1 in 1000 cases. Immunocompromised patients can also present with severe pneumonitis and without the classical viral prodrome.
Immune amnesia, caused by depletion of B-cell and T-cell memory by the measles virus in unvaccinated patients infected with the measles virus, may last up to 1 year in fully recovered patients and increase susceptibility to sometimes severe secondary infections, particularly pneumonia.
Historically, late complications in underresourced settings have included malnutrition and blindness.
Subacute sclerosing panencephalitis (SSPE) is a delayed neurodegenerative disorder occurring approximately 10-11 years after acute infection. This complication is characterized by changes in personality, seizures, and coma and eventuates in death.
Modified measles syndrome occurs in both fully vaccinated and undervaccinated individuals. Patients who fail to respond to the measles vaccine are at risk of measles infection due to primary vaccine failure. Secondary vaccine failure occurs when patients who have responded to the vaccine have waning immunity over time and experience breakthrough infection with milder symptoms, a lower viral load, and a lower risk for transmission.
Although measles was declared eliminated in the United States in 2000, outbreaks continue to occur and appear to be on the rise since 2023. While most cases have been associated with importation of measles by unvaccinated international travelers resulting in local outbreaks in communities with clusters of unvaccinated individuals, current measles, mumps, and rubella (MMR) vaccination coverage among US kindergartners is now below the 95% coverage target (and much lower in some communities) that helped achieve disease "elimination," and the risk for a return to domestic spread is growing.
Per the CDC, as of December 3, 2025, a total of 1828 confirmed measles cases have been reported from 43 jurisdictions in the United States. There have been 46 outbreaks (defined as 3 or more related cases) reported in 2025, and 87% of confirmed cases (1597 of 1828) are outbreak-associated. (For comparison, 16 outbreaks were reported during 2024, and 69% of cases [198 of 285] were outbreak-associated.) There are 3 confirmed deaths. Refer to the CDC for the latest information on measles cases and outbreaks in the United States.
Related topic: atypical measles syndrome (occurs in those receiving formalin-inactivated measles vaccine between 1963 and 1967 or in whom immunization has failed; will spread from the extremities inward; petechiae, purpura, vesicles, or acral edema can occur; cough and conjunctivitis are not as marked as in classic measles).
Measles is transmitted via respiratory droplets and can remain viable and transmissible for up to 2 hours in an airspace after an infected person leaves an area. The incubation period after the measles virus enters the upper respiratory mucosa is about 10 days (range 7-21 days), with the rash typically appearing about 14 days after an exposure. Infected individuals are considered contagious from about 4 days prior to the appearance of the rash through about 4 days after its appearance.
A prodrome characterized by fever (up to 40.5°C [105°F]), coryza (nasal congestion), cough, and conjunctivitis occurs for about 3-4 days followed by the onset of the rash (sometimes immunocompromised individuals do not develop the rash or develop a rash with severe desquamation). The coryza, a "barking" cough, and conjunctivitis will increase in severity until the rash reaches its peak. The US Centers for Disease Control and Prevention (CDC) reports that approximately 1 in 10 children with measles will develop otitis media, and up to 1 in 20 will develop pneumonia. Encephalitis is a complication in about 1 in 1000 cases. Immunocompromised patients can also present with severe pneumonitis and without the classical viral prodrome.
Immune amnesia, caused by depletion of B-cell and T-cell memory by the measles virus in unvaccinated patients infected with the measles virus, may last up to 1 year in fully recovered patients and increase susceptibility to sometimes severe secondary infections, particularly pneumonia.
Historically, late complications in underresourced settings have included malnutrition and blindness.
Subacute sclerosing panencephalitis (SSPE) is a delayed neurodegenerative disorder occurring approximately 10-11 years after acute infection. This complication is characterized by changes in personality, seizures, and coma and eventuates in death.
Modified measles syndrome occurs in both fully vaccinated and undervaccinated individuals. Patients who fail to respond to the measles vaccine are at risk of measles infection due to primary vaccine failure. Secondary vaccine failure occurs when patients who have responded to the vaccine have waning immunity over time and experience breakthrough infection with milder symptoms, a lower viral load, and a lower risk for transmission.
Although measles was declared eliminated in the United States in 2000, outbreaks continue to occur and appear to be on the rise since 2023. While most cases have been associated with importation of measles by unvaccinated international travelers resulting in local outbreaks in communities with clusters of unvaccinated individuals, current measles, mumps, and rubella (MMR) vaccination coverage among US kindergartners is now below the 95% coverage target (and much lower in some communities) that helped achieve disease "elimination," and the risk for a return to domestic spread is growing.
Per the CDC, as of December 3, 2025, a total of 1828 confirmed measles cases have been reported from 43 jurisdictions in the United States. There have been 46 outbreaks (defined as 3 or more related cases) reported in 2025, and 87% of confirmed cases (1597 of 1828) are outbreak-associated. (For comparison, 16 outbreaks were reported during 2024, and 69% of cases [198 of 285] were outbreak-associated.) There are 3 confirmed deaths. Refer to the CDC for the latest information on measles cases and outbreaks in the United States.
Related topic: atypical measles syndrome (occurs in those receiving formalin-inactivated measles vaccine between 1963 and 1967 or in whom immunization has failed; will spread from the extremities inward; petechiae, purpura, vesicles, or acral edema can occur; cough and conjunctivitis are not as marked as in classic measles).
Codes
ICD10CM:
B05.9 – Measles without complication
SNOMEDCT:
14189004 – Measles
B05.9 – Measles without complication
SNOMEDCT:
14189004 – Measles
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/25/2026
Last Updated:03/23/2026
Last Updated:03/23/2026
 Patient Information for Measles in Adult
Patient Information for Measles in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Measles in Adult