The estimated annual incidence of morphea is 3.4-27 cases per 100 000. Morphea occurs in all races and ethnicities, although White individuals seem to be most frequently affected. A family history of connective tissue or autoimmune diseases is more likely in an individual with morphea. Up to 20% of patients with morphea have a concomitant autoimmune disease such as psoriasis, vitiligo, inflammatory bowel disease (Crohn disease, ulcerative colitis), diabetes mellitus, and thyroiditis.
Morphea can be classified into 5 main types (limited, generalized, linear, deep, and mixed), as well as several clinical subtypes (eg, plaque-type, pansclerotic, linear, en coup de sabre). Eosinophilic fasciitis, also known as Shulman syndrome, is often considered a part of the clinical spectrum of morphea.
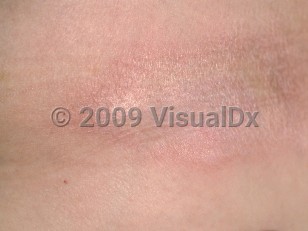
Plaque-type morphea is the most common form of localized scleroderma in adults. In plaque-type morphea, round or oval plaques are localized to 1 or 2 cutaneous sites. Lesions are usually asymmetrically distributed and can be associated with alopecia and decreased sweat production. Concomitant genital lichen sclerosus may be present in up to 40% of patients with plaque-type morphea.
In the linear subtype, there is band-like cutaneous sclerosis that is usually unilateral and can cause contractures and limb-length discrepancies in up to 10% of patients. En coup de sabre is a specific subtype of linear morphea that affects the paramedian forehead and scalp, and it can be accompanied by alopecia as well as ocular, neurologic, and odontostomatologic complications. Progressive facial hemiatrophy, also known as Parry-Romberg syndrome, is characterized by minimal cutaneous changes with significant unilateral atrophy of the underlying tissue of the face, often with underlying cranial abnormalities and increased risk of seizures.
Generalized morphea is a rare variant that is defined as more than 4 plaques larger than 3 cm and/or involving 2 or more body sites. This subtype is predominant in women. Individuals with this variant are more likely to have systemic symptoms including myalgias, arthralgias, and fatigue.
Pansclerotic morphea is a debilitating variant that affects subcutaneous tissues and even bone. There is associated muscle atrophy, joint contractures, and nonhealing ulcers.
Complications include:
- Joint mobility and impairment of muscle growth – in linear or deep morphea crossing joint lines
- Ocular or oral complications – in craniofacial morphea
- Carpal tunnel syndrome – in morphea at the wrist
- Chronic ulcers or squamous cell carcinoma – in pansclerotic morphea