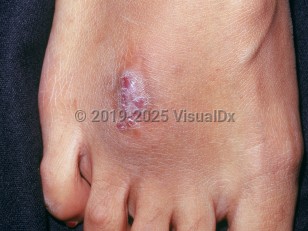
Mycetoma
Alerts and Notices
Important News & Links
Synopsis

Mycetoma (also known as Madura foot) is a chronic, slowly progressive infection of the skin and subcutaneous tissue, typically resulting from traumatic inoculation of diverse groups of microorganisms. The causative agents are found in hot and humid climate regions in the soil, plants, woods, and decaying plant materials, and they belong to different genera of fungus (eumycetoma) or bacteria (actinomycetoma). Over 55 microorganisms are identified as causative agents, with Madurella mycetomatis, Acremonium, Fusarium, and Aspergillus species as the most common causative agents for eumycetoma, while Streptomyces somaliensis and Nocardia brasiliensis are the most common causative organisms for actinomycetoma. The geographic distribution of causative organisms varies, with eumycetoma most common in Africa and India, and actinomycetoma more prevalent in Latin America.
Mycetoma is primarily diagnosed in tropical, subtropical, and equatorial regions, predominantly affecting poor and marginalized populations with limited access to medical care. In 2017, the World Health Organization (WHO) categorized mycetoma as a Neglected Tropical Disease. Risk factors for mycetoma include trauma, skin exposure to soil and vegetation, male sex, and immunodeficiency. Studies have shown that more than 90% of cases occur in individuals older than 18 years. In about 85% of cases, mycetomas occur on the feet and lower extremities, where trauma and subsequent soil exposure are most likely. Mycetomas have been reported on other body areas less commonly (eg, hands, thighs, buttocks, forearms, shoulders, and head and neck).
After initial exposure to the pathologic organism, there is an incubation period of months to years. The time from initial manifestation to consultation is reported to range from 3 months to 50 years.
The clinical course is determined by the causative organism, the site of the lesion, and host factors. Actinomycetoma is more destructive, progresses rapidly, and invades bone earlier than eumycetoma. Most infections remain localized and may cause significant local destruction. Spread of infection can occur locally in a sporotrichoid distribution to the nearby lymphatic vessels and lymph nodes. Hematologic spread has also been demonstrated. Poorer prognosis may be associated with head and upper thigh lesions because they may extend intracranially and to visceral organs.
Related topic: actinomycosis
Mycetoma is primarily diagnosed in tropical, subtropical, and equatorial regions, predominantly affecting poor and marginalized populations with limited access to medical care. In 2017, the World Health Organization (WHO) categorized mycetoma as a Neglected Tropical Disease. Risk factors for mycetoma include trauma, skin exposure to soil and vegetation, male sex, and immunodeficiency. Studies have shown that more than 90% of cases occur in individuals older than 18 years. In about 85% of cases, mycetomas occur on the feet and lower extremities, where trauma and subsequent soil exposure are most likely. Mycetomas have been reported on other body areas less commonly (eg, hands, thighs, buttocks, forearms, shoulders, and head and neck).
After initial exposure to the pathologic organism, there is an incubation period of months to years. The time from initial manifestation to consultation is reported to range from 3 months to 50 years.
The clinical course is determined by the causative organism, the site of the lesion, and host factors. Actinomycetoma is more destructive, progresses rapidly, and invades bone earlier than eumycetoma. Most infections remain localized and may cause significant local destruction. Spread of infection can occur locally in a sporotrichoid distribution to the nearby lymphatic vessels and lymph nodes. Hematologic spread has also been demonstrated. Poorer prognosis may be associated with head and upper thigh lesions because they may extend intracranially and to visceral organs.
Related topic: actinomycosis
Codes
ICD10CM:
B47.9 – Mycetoma, unspecified
SNOMEDCT:
410039003 – Mycetoma
B47.9 – Mycetoma, unspecified
SNOMEDCT:
410039003 – Mycetoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:03/18/2024
Last Updated:04/02/2024
Last Updated:04/02/2024
Mycetoma