MAI can be isolated from many environmental sources including soil and water. Transmission of the pathogen is thought to be due to inhalation or ingestion of the organism (inhalation for pulmonary disease). Using nucleic acid analysis, microbiology laboratories are now able to routinely identify the specific species (M avium or M intracellulare) causing infection. Certain serovars are felt to be more virulent than others.
In the United States, most cases of pulmonary MAI infection occur in women. The average age at diagnosis is 60. Patients with chronic obstructive pulmonary disease (COPD) or who are immunocompromised are at increased risk for this infection.
The incubation period is not known, but in many cases, symptoms progress slowly over months or years prior to diagnosis. The presentation of MAI pulmonary disease varies. On one end of the spectrum are thin, elderly, white women presenting with the "Lady Windermere syndrome." These patients may not have a previous history of lung disease. They present with a productive cough that is usually long-standing (present for months). They may complain of fatigue. Fever and hemoptysis are not common. The chest x-ray may show a nodular-bronchiectatic pattern or fibrocavitary disease (cavities are present only about 25% of the time). Tree-in-bud opacities are also commonly seen.
On the other end of the spectrum are patients who typically have a history of smoking or other lung disease and present with more severe symptoms. Lung involvement in these patients is more extensive, with a high rate of cavitary lung lesions. Many patients will have bilateral lung disease. MAI infection in this population may also be associated with fever and weight loss.
The evolution of symptoms varies. In many patients with Lady Windermere syndrome, symptoms may remain stable or may slowly worsen over the course of months to years.
MAI lung disease may occasionally present as a solitary pulmonary nodule and may require biopsy for diagnosis.
MAI has also been associated with a hypersensitivity pneumonitis in patients using hot tubs. These patients present with dry cough and dyspnea. Some have fever. Chest imaging is not specific. The most common chest x-ray finding in one series was diffuse nodular or interstitial infiltrates.
Culture of the organism from sputum does not imply that the organism is causing infection, as colonization with MAI has been well described. Patients with cystic fibrosis, for example, have a high rate of colonization with nontuberculous mycobacteria. A combination of symptoms, radiography, and culture is necessary to make the diagnosis. In addition, not all patients diagnosed with MAI lung disease require antibiotic therapy. Consultation with an expert in infectious diseases or pulmonary medicine is frequently helpful prior to starting treatment for MAI lung disease.
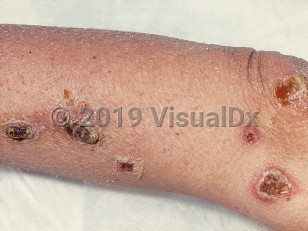
In addition to pulmonary infection, MAI infection can also result in disseminated disease (usually in patients with AIDS), cervical lymphadenitis, tenosynovitis, and cutaneous infection.
Three clinical forms of infection are seen:
- Primary post-traumatic inoculation (which is rare and usually seen in immunocompetent persons) – Most cases have been seen in children aged 2-10 years and do not progress to systemic disease.
- Disseminated systemic disease (DMAI) is most often seen in the immunocompromised patient and commonly involves the lungs, lymph nodes, liver, spleen, bone marrow, and skin. The patient may have fever, pulmonary symptoms, lymphadenopathy, hepatosplenomegaly, weight loss, and fatigue. Untreated DMAI is associated with increased mortality.
- Cervical adenitis in children (median age 3 years) is most commonly caused by MAI, having an indolent course and causing local destruction but only rarely disseminating.