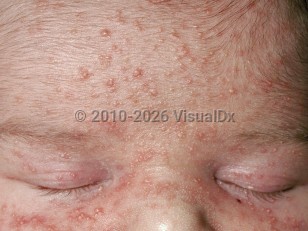
Neonatal acne
Alerts and Notices
Important News & Links
Synopsis

This summary discusses acne in neonates. Infantile acne and acne vulgaris in adults and children are addressed separately.
Neonatal acne, or neonatal cephalic pustulosis, is a very common acneiform eruption occurring on the face of neonates (ages 0-6 weeks). Many separate these two conditions as neonatal cephalic pustulosis for a solely papulopustular eruption, often associated with Malassezia species, and neonatal acne for eruptions that include open comedones or nodulocystic lesions. Both tend to be very mild and spontaneously resolve by age 3-6 months without residual sequelae.
Neonatal acne, or neonatal cephalic pustulosis, is a very common acneiform eruption occurring on the face of neonates (ages 0-6 weeks). Many separate these two conditions as neonatal cephalic pustulosis for a solely papulopustular eruption, often associated with Malassezia species, and neonatal acne for eruptions that include open comedones or nodulocystic lesions. Both tend to be very mild and spontaneously resolve by age 3-6 months without residual sequelae.
Codes
ICD10CM:
L70.4 – Infantile acne
SNOMEDCT:
49706007 – Neonatal acne
L70.4 – Infantile acne
SNOMEDCT:
49706007 – Neonatal acne
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/29/2025
Last Updated:10/29/2025
Last Updated:10/29/2025
 Patient Information for Neonatal acne
Patient Information for Neonatal acne
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Neonatal acne