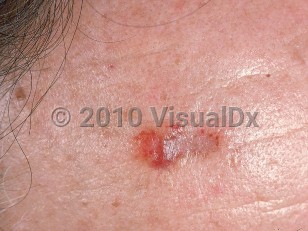
Nodular amyloidosis
Alerts and Notices
Important News & Links
Synopsis

Nodular amyloidosis is an uncommonly encountered form of primary cutaneous amyloidosis (a category which also includes lichen and macular amyloidosis, poikiloderma-like cutaneous amyloidosis, primary cutaneous amyloidosis of the auricular concha, and the exceedingly rare entity of amyloidosis cutis dyschromica). In nodular amyloidosis, the material deposited in the dermis is thought to be derived from immunoglobulin light chains or beta-2 microglobulin produced by plasma cells in the lesions. This is in contrast to macular and lichen amyloidosis, in which the material deposited in the dermis is derived from keratin.
In nodular amyloidosis, the amyloid deposits are found in the dermis and subcutaneous fat and within the walls of blood vessels. Clinically, the condition presents as brownish-pink, waxy-appearing papules or nodules, occurring singly or in groups, most commonly on acral surfaces and the face. Involvement of the trunk, genitals, and extremities has also been reported. There can be telangiectasias or atrophy of the overlying epidermis.
Men and women are affected equally. The disease usually begins in middle age. Typically, the prognosis is quite good, although a small minority of people (less than 10%) progress to systemic amyloidosis. A significant number of cases of nodular amyloidosis have occurred in association with Sjögren syndrome. For this reason, a thorough history and physical examination as well as appropriate screening tests to exclude this autoimmune disease are necessary.
In nodular amyloidosis, the amyloid deposits are found in the dermis and subcutaneous fat and within the walls of blood vessels. Clinically, the condition presents as brownish-pink, waxy-appearing papules or nodules, occurring singly or in groups, most commonly on acral surfaces and the face. Involvement of the trunk, genitals, and extremities has also been reported. There can be telangiectasias or atrophy of the overlying epidermis.
Men and women are affected equally. The disease usually begins in middle age. Typically, the prognosis is quite good, although a small minority of people (less than 10%) progress to systemic amyloidosis. A significant number of cases of nodular amyloidosis have occurred in association with Sjögren syndrome. For this reason, a thorough history and physical examination as well as appropriate screening tests to exclude this autoimmune disease are necessary.
Codes
ICD10CM:
E85.9 – Other amyloidosis
SNOMEDCT:
733729003 – Primary localized cutaneous amyloidosis
E85.9 – Other amyloidosis
SNOMEDCT:
733729003 – Primary localized cutaneous amyloidosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:02/06/2020
Last Updated:05/11/2020
Last Updated:05/11/2020