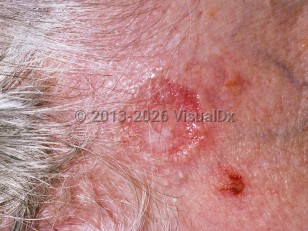
Nodular basal cell carcinoma - Anogenital in
See also in: Overview,External and Internal Eye,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

There are many subtypes of BCC, including nodular, superficial, infundibulocystic, fibroepithelial, morpheaform (sclerosing, desmoplastic), infiltrative, micronodular, and basosquamous. Nodular BCC is the most common subtype overall and accounts for half of all lesions. In Black and Hispanic patients, BCCs are more often pigmented BCCs.
The most prevalent risk factor contributing to the development of BCCs is sun exposure. Other risk factors for BCCs include environmental exposure (ie, ionizing radiation, indoor tanning, chemicals such as arsenic, psoralen plus UVA, and coal tar), phenotype (freckling, red hair, light skin that always burns and never tans), immunosuppression such as organ transplantation (which results in a 5-10 times higher risk of BCCs than the general population), and various genetic syndromes including xeroderma pigmentosum, oculocutaneous albinism, Muir-Torre syndrome, basal cell nevus syndrome (Gorlin syndrome), Rombo syndrome, and Bazex-Dupré-Christol syndrome. The gene most frequently altered in BCCs is the PTCH1 gene, followed by the TP53 gene.
Although BCCs typically arise in hair-bearing areas, they can rarely be seen in hairless genital mucosa for an unknown reason. BCC of the vulva is exceedingly rare and defies conventional understanding of the disease, as this area is unlikely to receive much sun exposure and BCCs on this area arise even on non-hair-bearing skin.
Although BCCs are almost never fatal, local tissue destruction and disfiguration occur. The metastasis rate of BCCs is approximately 1 in 35 000. Metastasis is rare and typically occurs through perineural spread, lymph node metastasis, and then lung / bone metastasis.
Codes
C44.91 – Basal cell carcinoma of skin, unspecified
SNOMEDCT:
403911008 – Nodulo-ulcerative basal cell carcinoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:04/30/2024
 Patient Information for Nodular basal cell carcinoma - Anogenital in
Patient Information for Nodular basal cell carcinoma - Anogenital in - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient