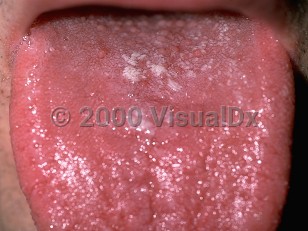
Oral candidiasis in Child
See also in: Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Although not common in children over the age of 12 months, it may occur in children who are on antibiotics, who have an underlying endocrine disorder (eg, type 1 diabetes mellitus), or who are immunosuppressed due to primary immunodeficiency disorders or secondary to malignancy, immunosuppressive medication, or human immunodeficiency virus (HIV) infection.
The child may be symptom free or may complain of a burning tongue and soreness or pain in the mouth or pain on swallowing.
Oral candidiasis occurs in children in three main clinical forms. The most common form in children is the pseudomembranous variety: white plaque formation typically appears on the tongue, lips, inner surface of the cheeks, and palate and can leave behind punctate bleeding and patches of reddened mucosa when scraped.
In children with HIV infection, oral thrush is the most common candidal infection. The presentation, however, differs, and these children may show signs of all of the types of mucous membrane infections.
Candida at the corners of the mouth is known as angular cheilitis or perlèche. Crusting, small ulcers, or fissures can be present at the angles of the mouth.
In median rhomboid glossitis, a smooth, red, diamond-shaped area is present on the dorsal surface of the tongue.
Related topic: Angular cheilitis
Codes
B37.0 – Candidal stomatitis
SNOMEDCT:
79740000 – Oral candidiasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:10/05/2017
 Patient Information for Oral candidiasis in Child
Patient Information for Oral candidiasis in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient