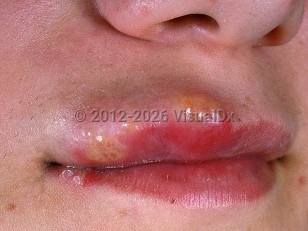
Orofacial herpes simplex virus in Adult
See also in: Oral Mucosal LesionAlerts and Notices
Important News & Links
Synopsis

Orofacial herpes simplex virus (HSV) infections are common and should be considered within the differential diagnosis of a patient presenting with facial vesicles or crusts, or alternatively, intraoral vesicles, erosions, or ulcers. Although this is usually an infection of herpes simplex virus type 1 (HSV-1), orofacial infection can be caused by herpes simplex virus type 2 (HSV-2). Oral infection with HSV-2 is more frequent in patients with HIV. Either virus may be involved in genital infections.
HSV is highly contagious. It is spread by direct contact with the lesions. Primary herpetic gingivostomatitis is an acute infection of the oral mucous membranes by HSV that results from initial exposure to the virus. Most primary exposures (approximately 90%) are subclinical and asymptomatic. Herpetic gingivostomatitis occurs most often in children aged between 10 months and 5 years, but it can occur at any age. Patients experience a flu-like illness with fever, loss of appetite, malaise, and lymphadenopathy. Painful mouth sores and a sore throat develop, and difficulty eating and swallowing places the patients at risk for dehydration. The systemic and oral signs and symptoms develop within days of each other.
The virus establishes lifelong latency, and both asymptomatic reactivation, as well as recrudescence, are common. In recrudescence, patients report a prodrome of burning, itching, and a tingling sensation before the actual lesions appear. HSV recrudescence on the lips is also known as cold sores, fever blisters, or herpes labialis; inside the mouth, lesions only occur on the keratinized tissues of the tongue dorsum, hard palatal mucosa, and gingiva in healthy hosts, but they may occur on any surface in the immunocompromised host. Intraoral involvement in recrudescent disease in immunocompetent hosts is rare.
HSV can also disseminate, occurring on skin areas distant from the lips. Two general groups of patients are at risk of developing disseminated HSV: patients with underlying skin disease and immunocompromised patients. Pregnant individuals with primary HSV infection are at increased risk for severe illness, ie, dissemination and hepatitis, particularly in the third trimester.
Localized HSV in areas other than the face and mouth, such as herpetic whitlow, are discussed separately. Other related topics include HSV blepharitis, HSV conjunctivitis, HSV encephalitis, HSV gladiatorum, HSV keratitis, HSV pneumonia, and neonatal HSV.
HSV is highly contagious. It is spread by direct contact with the lesions. Primary herpetic gingivostomatitis is an acute infection of the oral mucous membranes by HSV that results from initial exposure to the virus. Most primary exposures (approximately 90%) are subclinical and asymptomatic. Herpetic gingivostomatitis occurs most often in children aged between 10 months and 5 years, but it can occur at any age. Patients experience a flu-like illness with fever, loss of appetite, malaise, and lymphadenopathy. Painful mouth sores and a sore throat develop, and difficulty eating and swallowing places the patients at risk for dehydration. The systemic and oral signs and symptoms develop within days of each other.
The virus establishes lifelong latency, and both asymptomatic reactivation, as well as recrudescence, are common. In recrudescence, patients report a prodrome of burning, itching, and a tingling sensation before the actual lesions appear. HSV recrudescence on the lips is also known as cold sores, fever blisters, or herpes labialis; inside the mouth, lesions only occur on the keratinized tissues of the tongue dorsum, hard palatal mucosa, and gingiva in healthy hosts, but they may occur on any surface in the immunocompromised host. Intraoral involvement in recrudescent disease in immunocompetent hosts is rare.
HSV can also disseminate, occurring on skin areas distant from the lips. Two general groups of patients are at risk of developing disseminated HSV: patients with underlying skin disease and immunocompromised patients. Pregnant individuals with primary HSV infection are at increased risk for severe illness, ie, dissemination and hepatitis, particularly in the third trimester.
Localized HSV in areas other than the face and mouth, such as herpetic whitlow, are discussed separately. Other related topics include HSV blepharitis, HSV conjunctivitis, HSV encephalitis, HSV gladiatorum, HSV keratitis, HSV pneumonia, and neonatal HSV.
Codes
ICD10CM:
B00.2 – Herpesviral gingivostomatitis and pharyngotonsillitis
SNOMEDCT:
235055003 – Oral herpes simplex infection
B00.2 – Herpesviral gingivostomatitis and pharyngotonsillitis
SNOMEDCT:
235055003 – Oral herpes simplex infection
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/26/2022
Last Updated:12/08/2022
Last Updated:12/08/2022
 Patient Information for Orofacial herpes simplex virus in Adult
Patient Information for Orofacial herpes simplex virus in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Orofacial herpes simplex virus in Adult
See also in: Oral Mucosal Lesion