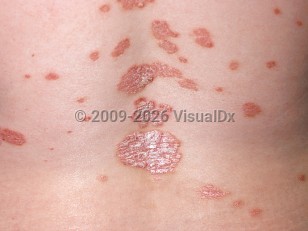
Psoriasis in Child
See also in: Anogenital,Hair and Scalp,Nail and Distal DigitAlerts and Notices
Important News & Links
Synopsis

Psoriasis is a polygenic disease, and several psoriasis susceptibility genes have been identified over recent years. Certain individuals with genetic susceptibility develop a psoriatic phenotype after exposure to environmental triggers such as infection, medications, and medical comorbidities, among others. Aberrant T-cell function and keratinocyte responses are believed to be major culprits in the pathogenesis of psoriasis.
Psoriasis is fairly common in childhood but may occur in infancy (see infantile psoriasis). It occurs worldwide and is estimated to affect 1%-3% of the population, with 20% of cases presenting before age 20 years.
Several clinical patterns exist, and multiple forms may be observed in a single patient. Typical plaque-type psoriasis (psoriasis vulgaris) is discussed here; other forms include guttate psoriasis (commonly seen in children and adolescents, often following an upper respiratory tract infection, usually streptococcal pharyngitis); palmoplantar psoriasis; erythrodermic psoriasis; and pustular psoriasis. Inverse psoriasis occurs in intertriginous or flexural areas of the body, such as the axillae, groin, genitals, inframammary areas, face, and eyelids. Linear psoriasis is a rare variant that is characterized by the distribution of psoriatic lesions along the lines of Blaschko. The pathogenesis remains unclear, but it seems to be related to genetic mosaicism.
Pediatric psoriasis may present as well-demarcated erythematous plaques limited to one body area (eg, the face, nails, genitals, scalp, feet, or even a solitary fingertip). Fingernails are more often involved compared to toenails in children. In one study, nail pitting was mostly seen in fingernails, while toenails exhibited onycholysis and paronychia. A review of pediatric psoriasis found that scalp psoriasis was more common in female patients, while nail involvement was more common in male patients, suggesting a possible role of chronic incidental trauma in these locations.
The prevalence of psoriatic arthritis in individuals with psoriasis is estimated at around 17%. It more commonly affects adults compared to children. Individuals with nail involvement seem to be at increased risk for developing this erosive seronegative arthritis, which can be a source of considerable morbidity. In addition, the presence of psoriatic arthritis has been associated with higher severity score for nail psoriasis. Warning signs of psoriatic arthritis include tender, swollen joints that may be warm to the touch or painful swelling of the fingers.
Comorbidities may include hypertension, obesity, hyperlipidemia, diabetes mellitus, steatotic liver disease, cardiovascular disease, cerebrovascular disease, Crohn disease, ulcerative colitis, rheumatologic disease, juvenile idiopathic arthropathy, depression, anxiety, bipolar disorder, substance abuse, and eating disorders.
Immunocompromised states can trigger psoriasis flares with widespread lesions. For example, patients with HIV have a ninefold increased risk of active disease when CD4 counts fall below 200, and more than 80% experience recurrence of psoriatic lesions when CD4 counts drop under 450.
The National Psoriasis Foundation is an excellent resource for patients: www.psoriasis.org.
Codes
L40.0 – Psoriasis vulgaris
SNOMEDCT:
9014002 – Psoriasis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:08/24/2025
 Patient Information for Psoriasis in Child
Patient Information for Psoriasis in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient