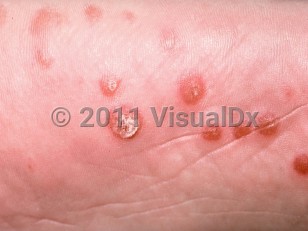
Reactive arthritis - Nail and Distal Digit
See also in: Overview,AnogenitalAlerts and Notices
Important News & Links
Synopsis

Reactive arthritis (previously called Reiter syndrome) is a type of seronegative spondyloarthropathy that affects large joints of the lower extremities, typically 1-4 weeks following an episode of enteritis or urethritis. It is called "reactive" as opposed to "septic" because the arthritis is sterile; bacteria provoke the arthritis without directly invading the joint space. Typically, fewer than 5 joints are affected and it presents as acutely painful oligoarthritis. Patients can also complain of stiffness and pain of the lower back. Enthesitis is especially common, and dactylitis (sausage digits) can also be seen. Patients occasionally have systemic features, including fever, weight loss, and fatigue. Only a minority of patients present with the classic triad of arthritis, urethritis, and conjunctivitis.
Reactive arthritis may rarely occur in children; it is termed epidemic or post-dysenteric. In adults, it is termed epidemic or venereal. It was initially described after infections with specific bacteria: Chlamydia trachomatis, Shigella, Salmonella, Yersinia, and Campylobacter. However, recent studies have implicated Clostridioides difficile, Giardia, and other atypical infections as triggers for ReA. Chlamydia trachomatis is the most common trigger and it may be asymptomatic in 10% of patients. It is unclear how infections trigger the disease. When reactive arthritis is secondary to a gastrointestinal infection, it affects both sexes equally. However, reactive arthritis secondary to C trachomatis infection is more common in men. Those patients who are positive for human immunodeficiency virus (HIV) or human leukocyte antigen (HLA)-B27 typically have more severe arthritis.
Nail involvement affects 20%-30% of patients with reactive arthritis. Changes resemble those of nail psoriasis including onycholysis, nail pitting, subungual hyperkeratosis, and pustules affecting the nail folds. Paronychia is also common. Other reported findings are ridging, splitting, elkonyxis (loss of nail plate substance above the lunula only), and brown-red discoloration.
For most patients, reactive arthritis is a self-limited disease and they recover completely within 2-6 months. A chronic arthritis may persist in a minority, usually in association with HLA-B27 phenotype. Other patients can develop recurrent episodes of reactive arthritis after encountering the same organism.
Reactive arthritis may rarely occur in children; it is termed epidemic or post-dysenteric. In adults, it is termed epidemic or venereal. It was initially described after infections with specific bacteria: Chlamydia trachomatis, Shigella, Salmonella, Yersinia, and Campylobacter. However, recent studies have implicated Clostridioides difficile, Giardia, and other atypical infections as triggers for ReA. Chlamydia trachomatis is the most common trigger and it may be asymptomatic in 10% of patients. It is unclear how infections trigger the disease. When reactive arthritis is secondary to a gastrointestinal infection, it affects both sexes equally. However, reactive arthritis secondary to C trachomatis infection is more common in men. Those patients who are positive for human immunodeficiency virus (HIV) or human leukocyte antigen (HLA)-B27 typically have more severe arthritis.
Nail involvement affects 20%-30% of patients with reactive arthritis. Changes resemble those of nail psoriasis including onycholysis, nail pitting, subungual hyperkeratosis, and pustules affecting the nail folds. Paronychia is also common. Other reported findings are ridging, splitting, elkonyxis (loss of nail plate substance above the lunula only), and brown-red discoloration.
For most patients, reactive arthritis is a self-limited disease and they recover completely within 2-6 months. A chronic arthritis may persist in a minority, usually in association with HLA-B27 phenotype. Other patients can develop recurrent episodes of reactive arthritis after encountering the same organism.
Codes
ICD10CM:
M02.30 – Reiter's disease, unspecified site
SNOMEDCT:
67224007 – Reactive arthritis
M02.30 – Reiter's disease, unspecified site
SNOMEDCT:
67224007 – Reactive arthritis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:10/17/2017
Last Updated:10/16/2022
Last Updated:10/16/2022
 Patient Information for Reactive arthritis - Nail and Distal Digit
Patient Information for Reactive arthritis - Nail and Distal Digit
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Reactive arthritis - Nail and Distal Digit
See also in: Overview,Anogenital