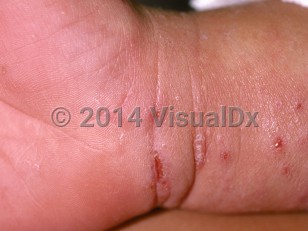
Scabies
See also in: AnogenitalAlerts and Notices
Important News & Links
Synopsis

This summary discusses adult patients. Scabies in children is addressed separately.
Scabies is an intensely pruritic eruption caused by the mite Sarcoptes scabiei var. hominis. It is transmitted most often via direct person-to-person contact and less frequently by fomites. It is extremely contagious, spreading between individuals who share close contact or living spaces. Prevalence rates are higher in children, residents of long-term care facilities, and sexually active persons, although scabies can appear in individuals of all ages and socioeconomic groups. Factors that contribute to the persistence and spread of scabies are overcrowding, delays in diagnosis, and poor public health awareness. Outbreaks in health care facilities, such as nursing homes, can result in dozens of patients and staff becoming infected.
In a typical infestation, there are 10-20 mites. Most patients mount an intense hypersensitivity reaction to the mites, which burrow into and just below the stratum corneum of the epidermis. This results in a widespread and highly pruritic eruption. The hypersensitivity reaction usually develops 2-6 weeks after initial infestation. Without medical treatment, the condition persists because the mites lay eggs, causing continued infestation. Scabies can cause a generalized eruption resembling erythroderma in the elderly, the institutionalized, and patients with immunosuppression or neurologic dysfunction (crusted scabies). In these patients, the mite burden is much higher, with thousands to millions of mites present on affected skin.
Scabies is an intensely pruritic eruption caused by the mite Sarcoptes scabiei var. hominis. It is transmitted most often via direct person-to-person contact and less frequently by fomites. It is extremely contagious, spreading between individuals who share close contact or living spaces. Prevalence rates are higher in children, residents of long-term care facilities, and sexually active persons, although scabies can appear in individuals of all ages and socioeconomic groups. Factors that contribute to the persistence and spread of scabies are overcrowding, delays in diagnosis, and poor public health awareness. Outbreaks in health care facilities, such as nursing homes, can result in dozens of patients and staff becoming infected.
In a typical infestation, there are 10-20 mites. Most patients mount an intense hypersensitivity reaction to the mites, which burrow into and just below the stratum corneum of the epidermis. This results in a widespread and highly pruritic eruption. The hypersensitivity reaction usually develops 2-6 weeks after initial infestation. Without medical treatment, the condition persists because the mites lay eggs, causing continued infestation. Scabies can cause a generalized eruption resembling erythroderma in the elderly, the institutionalized, and patients with immunosuppression or neurologic dysfunction (crusted scabies). In these patients, the mite burden is much higher, with thousands to millions of mites present on affected skin.
Codes
ICD10CM:
B86 – Scabies
SNOMEDCT:
128869009 – Infestation caused by Sarcoptes scabiei var hominis
B86 – Scabies
SNOMEDCT:
128869009 – Infestation caused by Sarcoptes scabiei var hominis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/28/2022
Last Updated:01/08/2017
Last Updated:01/08/2017
 Patient Information for Scabies
Patient Information for Scabies
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today