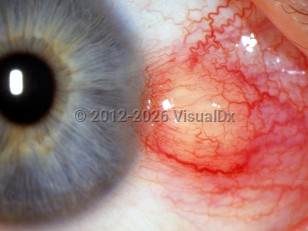
Sebaceous carcinoma
Alerts and Notices
Important News & Links
Synopsis

Sebaceous carcinoma (SC) is a rare malignant neoplasm that most commonly occurs on the eyelid but may also arise on extraocular skin. Periocular and extraocular tumors manifest differing genetic mutations and are classified separately. While the majority of individuals who develop SC are male, periocular SC occurs most frequently in females. Adults 60 and older are most commonly affected.
Periocular SC accounts for around 75% of all SCs. It is typically unilateral and arises more frequently from the upper than the lower eyelid, from the meibomian glands or the glands of Zeis. More rarely, it can arise from the eyebrow, caruncle, or lacrimal sac. Uncommonly, it can be multicentric and arise in both upper and lower eyelids. The presentation of eyelid tumors may be insidious, with cases masquerading as recurrent chalazia or blepharoconjunctivitis, leading to delayed diagnosis. The American Joint Committee on Cancer (AJCC) 8th edition staging system for eyelid carcinomas is employed for staging of periocular SC. The prognosis depends on the stage of the tumor, but T3 or other advanced tumors have the greatest mortality.
Extraocular SC occurs most frequently on the head or neck but may also arise from the trunk or extremities. Rare cases of the nasal vestibule have been reported.
Solid organ transplantation is a risk factor for SC. For periocular SC, a history of radiation therapy or the presence of lymphoma may also predispose. While some studies note no difference in 5-year survival rates for periocular and extraocular SC, others cite a higher mortality from eyelid tumors, especially if of the lower lid or with orbital extension. The Union for International Cancer Control TNM staging system 8th edition for skin carcinomas has been recommended for staging of extraocular SC.
While extraocular SC is strongly associated with Muir-Torre syndrome (MTS), sporadic periocular SC are not. MTS is an autosomal dominant condition of sebaceous tumors alongside with gastrointestinal, endometrial, urologic tumors.
Periocular SC accounts for around 75% of all SCs. It is typically unilateral and arises more frequently from the upper than the lower eyelid, from the meibomian glands or the glands of Zeis. More rarely, it can arise from the eyebrow, caruncle, or lacrimal sac. Uncommonly, it can be multicentric and arise in both upper and lower eyelids. The presentation of eyelid tumors may be insidious, with cases masquerading as recurrent chalazia or blepharoconjunctivitis, leading to delayed diagnosis. The American Joint Committee on Cancer (AJCC) 8th edition staging system for eyelid carcinomas is employed for staging of periocular SC. The prognosis depends on the stage of the tumor, but T3 or other advanced tumors have the greatest mortality.
Extraocular SC occurs most frequently on the head or neck but may also arise from the trunk or extremities. Rare cases of the nasal vestibule have been reported.
Solid organ transplantation is a risk factor for SC. For periocular SC, a history of radiation therapy or the presence of lymphoma may also predispose. While some studies note no difference in 5-year survival rates for periocular and extraocular SC, others cite a higher mortality from eyelid tumors, especially if of the lower lid or with orbital extension. The Union for International Cancer Control TNM staging system 8th edition for skin carcinomas has been recommended for staging of extraocular SC.
While extraocular SC is strongly associated with Muir-Torre syndrome (MTS), sporadic periocular SC are not. MTS is an autosomal dominant condition of sebaceous tumors alongside with gastrointestinal, endometrial, urologic tumors.
Codes
ICD10CM:
C44.131 – Sebaceous cell carcinoma of skin of unspecified eyelid, including canthus
D04.9 – Carcinoma in situ of skin, unspecified
SNOMEDCT:
307599002 – Sebaceous adenocarcinoma
C44.131 – Sebaceous cell carcinoma of skin of unspecified eyelid, including canthus
D04.9 – Carcinoma in situ of skin, unspecified
SNOMEDCT:
307599002 – Sebaceous adenocarcinoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:07/31/2024
Last Updated:05/24/2022
Last Updated:05/24/2022