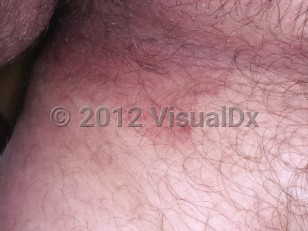
Tinea cruris in Adult
See also in: Cellulitis DDx,AnogenitalAlerts and Notices
Important News & Links
Synopsis

Tinea cruris (jock itch) is a superficial fungal infection of the skin of the groin area, most commonly caused by Trichophyton rubrum or other dermatophytes. Tinea cruris manifests as a symmetric erythematous rash on the inner thighs and the crural folds. It is frequently pruritic. People at higher risk include those who have diabetes mellitus, are obese, recently visited a tropical climate, wear tight-fitting or wet clothes (including bathing suits) for extended periods, share clothing with others, or participate in sports. It is often spread to the groin from a fungal infection of the feet (tinea pedis).
Tinea cruris is more common in postpubertal males. It rarely spreads to the penis, but if it does, it will be found only at the base of the penis.
Tinea cruris can be differentiated from cellulitis based on the location and the presence of scaling. In contrast to cellulitis, tinea cruris often occurs bilaterally.
In the immunocompromised patient, pruritus may be absent. There is an increased risk of all dermatophyte infections (tinea pedis, cruris, corporis, and faciale as well as Majocchi granuloma) in immunocompromised individuals.
A severe antifungal-resistant tinea has emerged in South Asia from the rapid spread of a novel dermatophyte species: Trichophyton indotineae. Terbinafine-resistant T indotineae infections have been reported in Asia, Europe, Canada, and the United States, including one case in New York City with no history of recent international travel.
Tinea cruris is more common in postpubertal males. It rarely spreads to the penis, but if it does, it will be found only at the base of the penis.
Tinea cruris can be differentiated from cellulitis based on the location and the presence of scaling. In contrast to cellulitis, tinea cruris often occurs bilaterally.
In the immunocompromised patient, pruritus may be absent. There is an increased risk of all dermatophyte infections (tinea pedis, cruris, corporis, and faciale as well as Majocchi granuloma) in immunocompromised individuals.
A severe antifungal-resistant tinea has emerged in South Asia from the rapid spread of a novel dermatophyte species: Trichophyton indotineae. Terbinafine-resistant T indotineae infections have been reported in Asia, Europe, Canada, and the United States, including one case in New York City with no history of recent international travel.
Codes
ICD10CM:
B35.6 – Tinea cruris
SNOMEDCT:
399029005 – Tinea cruris
B35.6 – Tinea cruris
SNOMEDCT:
399029005 – Tinea cruris
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:05/24/2023
 Patient Information for Tinea cruris in Adult
Patient Information for Tinea cruris in Adult
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Tinea cruris in Adult
See also in: Cellulitis DDx,Anogenital