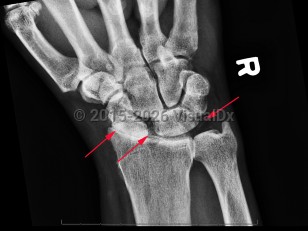
Calcium pyrophosphate deposition disease
Alerts and Notices
Important News & Links
Synopsis

CPPD disease usually affects patients 60 years and older and can have overlap with osteoarthritis. It affects women and men equally. Metabolic derangements such as hypophosphatemia, hypomagnesemia, and hypercalcemia increase the risk of CPPD. As such, conditions that predispose to metabolic derangements are associated with CPPD, such as hyperparathyroidism, hypothyroidism, Gitelman syndrome, hemochromatosis, and loop diuretic use. Similarly, inflammatory conditions of the joint can predispose to CPPD such as acute illness or joint trauma during the postoperative period, rheumatoid arthritis, and osteoarthritis.
While acute CPPD is more common and is often mistaken for gout, the less common chronic form of CPPD (<5% of cases of CPPD) can be mistaken for rheumatoid arthritis. Chronic CPPD often involves multiple joints, commonly involving the small peripheral joints of the arms and legs, often symmetrically. Inflammation can last for months but, unlike rheumatoid arthritis, inflammation of the affected joints can wax and wane independently of one another.
If the disease occurs in patients younger than 60, a familial history should be elicited as there are certain genetic associations that can cause earlier onset of disease.
The pathophysiology of pseudogout is not well understood, but CPP crystals forming in the cartilage is the first step in the disease process. Deposition of the CPP crystals affects the balance toward the production of pro-destructive prostaglandins and metalloproteinases, which destroy the chondrocytes and synoviocytes, cells that are important for the structural framework of cartilage and synovium.
Codes
E83.59 – Other disorders of calcium metabolism
SNOMEDCT:
239832006 – Calcium Pyrophosphate Deposition Disease
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/14/2017
 Patient Information for Calcium pyrophosphate deposition disease
Patient Information for Calcium pyrophosphate deposition disease - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient