Chronic mucocutaneous candidiasis is a genetic syndrome linked to defective cell-mediated immunity to Candida antigens and results in patients developing recurrent candidal infections of the skin, nails, and mucous membranes. Skin lesions appear as hyperkeratotic erythematous plaques. The affected nails are thickened, brittle, yellow-brown in color, and have associated paronychia. Most cases are seen in childhood and adolescence.
Cutaneous candidiasis includes the following:
- Generalized cutaneous candidiasis is an eruption of lesions covering the trunk, thorax, and extremities, which are accentuated in the genitocrural folds and around the anus, as well as the axilla, hands, and feet. Skin is erythematous, and lesions are initially discrete and then coalesce into larger lesions. Fissuring of the skin may be present.
- Intertrigo occurs at locations where the skin surfaces are closely apposed to each other. The most common sites are the axillary, inframammary, gluteal, and genitocrural regions. Intertrigo occurs due to widespread colonization, especially of macerated folds of moist skin. This usually presents as inflammation of the skin folds and starts as vesicles and pustules. The skin appears erythematous with surrounding vesicles and pustules.
- Candida miliaria affects the backs of bedridden patients with lesions in the form of vesicles and pustules.
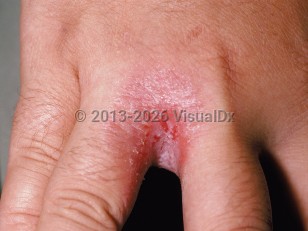
- Erosio interdigitalis blastomycetica is a candidal infection of the web spaces of the fingers and the toes. The skin lesions appear red and macerated and may extend onto the sites of the digits. Pustules may also be present. The toxic dermatitis initiated by Candida species is usually followed by infection with gram-negative rods exacerbating the chronicity of the lesion.
- Candida folliculitis is an infection of the hair follicles. Although usually localized, it may become widespread and must be differentiated from folliculitis due to dermatophytes and tinea versicolor.
- Candida balanitis is seen as vesicles on the penis that cause intense itching and burning. The lesions may also spread to the scrotum, thighs, and gluteal folds. See male genital candidiasis.
- Angular cheilitis can be caused by candidal infection of the angles of the mouth and results in macerated skin with deep creases and crust formation.
- Mammary candidiasis may occur during breastfeeding. It has a subtle presentation, with cracking and erythema of the nipple and surrounding areola. It may contribute to pain, burning, and discomfort with nursing. Often, oral thrush is noted in the nursing infant, which contributes to the development of mammary candidiasis.
Nosocomial infection with some Candida species (eg, Candida auris) has been associated with prolonged use of axillary temperature monitors.
Related topic: disseminated candidiasis (systemic candidiasis)



 Patient Information for
Patient Information for