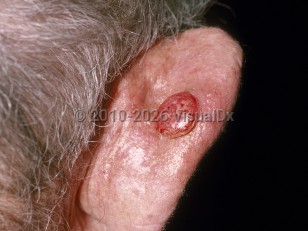
Cutaneous squamous cell carcinoma
See also in: Anogenital,Hair and Scalp,Nail and Distal DigitAlerts and Notices
Important News & Links
Synopsis

Light skin phototype is the most important factor related to developing SCC and is an independent predictor of the development of SCC in patients with solid organ transplantation. In individuals with darker skin phototypes, 30%-40% of SCCs develop within scars and chronic nonhealing ulcers (compared to 2% developing within such areas in people with lighter skin phototypes). SCC is the most common and second most common skin cancer in Black individuals and individuals of Hispanic descent, respectively.
A variety of other risk factors increase the likelihood of developing SCC. These include ultraviolet (UV) exposure, immunosuppression such as in individuals following solid organ transplantation (see skin cancer in organ transplant recipients) or individuals with HIV / AIDS, ionizing radiation exposure, cigarette smoking, human papillomavirus (HPV), chronic lymphocytic leukemia (CLL), family history of SCC, chemical exposure (eg, arsenic, mineral oil, coal tar, soot, mechlorethamine, polychlorinated biphenyls, and psoralen plus UVA treatment), freckling, red hair, and chronic nonhealing wounds. Approximately 10% of actinic keratoses (AKs) transform into skin cancer, with the most common being SCC. Furthermore, patients with AKs may be greater than 7 times more likely to develop SCC than patients without.
Dermatoses associated with a risk of SCC include discoid lupus erythematosus, lichen planus (ie, erosive, hypertrophic), and lichen sclerosus. A variety of genetic syndromes have also been associated with SCC. These include xeroderma pigmentosum, oculocutaneous albinism, epidermodysplasia verruciformis, dystrophic epidermolysis bullosa (recessive), Ferguson-Smith syndrome, and possibly Muir-Torre syndrome. Medications can also lead to the development of SCCs. Immunosuppressives, such as systemic immunomodulators or biologics, increase the risk of SCC, and the risk is proportional to length of therapy. Other implicated medications include voriconazole, thiopurine in patients with inflammatory bowel disease, immune checkpoint inhibitors (ICIs), BRAF V600 inhibitors such as vemurafenib and dabrafenib, and photosensitizing antihypertensive drugs such as alpha-2 receptor agonists and diuretics.
Drug-induced SCC and keratoacanthoma-like lesions are increasingly recognized in patients receiving oncologic therapies. With ICIs such as PD-1 and PD-L1 inhibitors, these lesions are most commonly attributed to immune reconstitution, leading to the unmasking of preexisting AKs or subclinical squamous proliferations. This immunologic mechanism predominates in ICI-associated cases and typically reflects enhanced immune surveillance rather than de novo tumorigenesis.
In contrast, BRAF inhibitors can induce paradoxical MAPK pathway activation, resulting in true de novo tumor formation, including SCCs and keratoacanthomas. Use of MEK inhibitors in combination with BRAF inhibitors mitigates this risk by suppressing downstream signaling.
Although SCC can arise on any skin surface including the mucosa, the most common areas of involvement are sun-exposed areas such as the head, neck, arms, and hands. The clinical presentation is highly variable among different demographic groups and tumor subtypes. Lesions may grow slowly or evolve rapidly.
The rate of metastasis is approximately 4%. The most common site of metastasis is the regional lymph node, but distal metastasis has been reported. Risk of metastasis is higher in immunosuppressed individuals, particularly solid organ transplant recipients, in primary lip lesions, and in non-UV-related SCCs.
Some features classify SCC as having a high risk of recurrence. These include aggressive histopathologic types (acantholytic, adenosquamous, carcinosarcomatous), depth greater than 2 mm, size larger than 2 cm, poorly defined borders, tumor arising in a site of prior radiation / burn or chronic inflammatory process, specific anatomic location (ie, tongue, vulva, penis), history of immunosuppression, moderate or poor differentiation on pathology, desmoplasia, and perineural or angiolymphatic invasion. These features may lead to selection of treatment options with lower recurrence rates, such as Mohs micrographic surgery (MMS), which has been shown to have lower recurrence rates than traditional wide local excision.
Various staging systems exist, although none is universally accepted. See Work Group. Guidelines of care for the management of cutaneous squamous cell carcinoma. J Am Acad Dermatol. 2018 Mar;78(3):560-578.
Related topics: oral squamous cell carcinoma, squamous cell carcinoma in situ
Codes
C44.92 – Squamous cell carcinoma of skin, unspecified
SNOMEDCT:
402815007 – Squamous cell carcinoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:09/30/2025
 Patient Information for Cutaneous squamous cell carcinoma
Patient Information for Cutaneous squamous cell carcinoma - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient