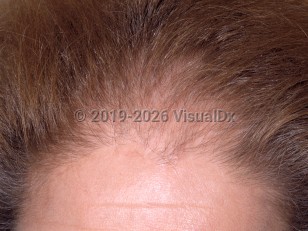
Female pattern alopecia, also known as androgenetic alopecia, is a common cause of nonscarring alopecia within the adult population, but it has also been reported in children and adolescents.
The youngest case of female pattern alopecia in the literature is a six-year-old female. Although data on prevalence is lacking, a retrospective study of 438 pediatric patients presenting with hair loss reported androgenetic alopecia as the second most common cause of alopecia in males and females after exclusion of tinea capitis diagnoses, with alopecia areata as the most prevalent diagnosis. However, in this case series, androgenetic alopecia surpassed alopecia areata as the most common cause of hair loss in the 12-19-year-old cohort (42% of 123 patients).
The pathophysiology of female pattern alopecia is poorly understood, and it is unclear how pathophysiology differs between pediatric and adult populations. The role of androgens in female pattern alopecia is less clear than that in male pattern alopecia, and the majority of females diagnosed with female pattern alopecia do not show biochemical or clinical signs of hyperandrogenism. Similarly, although genetics are believed to predispose patients to female pattern alopecia, the role of family history is less clear than that in male pattern alopecia. In the pediatric population, approximately 75% of patients with androgenetic alopecia have one parent with androgenetic alopecia and 25% have two parents with androgenetic alopecia.
The distribution of hair loss in female pattern alopecia is different than that in male pattern alopecia. Patients present with diffuse central thinning and widening of the middle part. This is described as a "Christmas tree pattern" when patients present with frontal accentuation. Patients may also present with bitemporal thinning. Frontotemporal recession and thinning at the vertex, as seen in male pattern alopecia, are less common. Areas of absolute baldness are also uncommon. Interestingly, both males and females in the pediatric population commonly present with the female pattern. In adolescence, male patients are more likely to present with the male pattern, although the female pattern can be seen. Pediatric patients with androgenetic alopecia often have other dermatologic diagnoses, such as acne and atopic dermatitis. Seborrheic dermatitis of the scalp is also commonly present in cases of androgenetic alopecia.
Female pattern alopecia in Child
Alerts and Notices
Important News & Links
Synopsis

Codes
ICD10CM:
L64.9 – Androgenic alopecia, unspecified
SNOMEDCT:
1108009 – Female pattern alopecia
L64.9 – Androgenic alopecia, unspecified
SNOMEDCT:
1108009 – Female pattern alopecia
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:01/09/2022
Last Updated:03/12/2024
Last Updated:03/12/2024
 Patient Information for Female pattern alopecia in Child
Patient Information for Female pattern alopecia in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Female pattern alopecia in Child