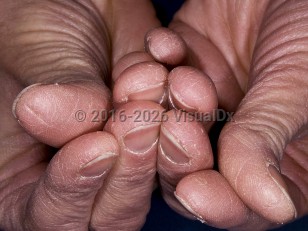
Irritant contact dermatitis in Child
See also in: External and Internal Eye,AnogenitalAlerts and Notices
Important News & Links
Synopsis

Irritant contact dermatitis should be differentiated from true allergic contact dermatitis, which is a delayed type-IV hypersensitivity (immune) reaction. Patients typically present complaining of a burning or stinging sensation early in the course of irritant contact dermatitis. Symptoms and a rash usually follow the exposure by hours if the irritant is strong; this is in contrast to allergic contact dermatitis, where symptoms are usually delayed by approximately 2 days following exposure. As the irritation becomes chronic and the skin continually inflamed, pruritus can become a predominant symptom.
Any body surface can be a location for irritant contact dermatitis. The hands are a common location in older children (see also hand dermatitis). The face and diaper area are commonly involved in younger children, such as in diaper dermatitis. Saliva in young babies who are teething or using bottles and pacifiers can cause irritant dermatitis on the cheeks and chin. Irritant dermatitis from cleansers used on toilet seats presents as dermatitis on the buttocks and posterior thighs.
Patients with a history of atopic dermatitis are particularly predisposed. Environmental factors include repeated exposure to water or frequent hand washing, hand sanitizers, soaps and solvents, fiberglass, mild acids, and alkalis. Dry air can also predispose to irritant contact dermatitis. Irritant contact dermatitis can occur at any age from infancy to adulthood.
Irritant contact dermatitis will improve when the child is no longer exposed to the irritant, such as a hand dermatitis that improves during summers and school breaks when a child is no longer using a particular hand sanitizer daily.
Codes
L24.9 – Irritant contact dermatitis, unspecified cause
SNOMEDCT:
110979008 – Primary irritant dermatitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:02/04/2021
 Patient Information for Irritant contact dermatitis in Child
Patient Information for Irritant contact dermatitis in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient