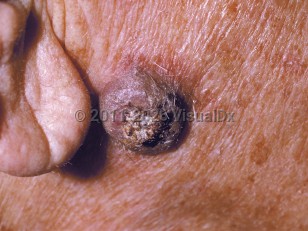
Keratoacanthomas are most commonly seen in individuals aged 60 years and older with light skin colors and a history of prolonged sun exposure. Men are more commonly affected than women.
Risk factors for keratoacanthomas include ultraviolet (UV) radiation, human papillomavirus infection, immunosuppression, and certain medications. Patients on immunosuppressant medications tend to have more persistent and chronic keratoacanthomas. Patients taking medications such as BRAF inhibitors or hedgehog inhibitors have also been reported to develop keratoacanthomas. Additionally, with anti-PD-1 / PD-L1 immunotherapy, rare cases of eruptive keratoacanthomas have been documented. Skin injury may also be a predisposing factor, and there are reports of keratoacanthomas developing in sites of prior trauma, in surgical scars, after laser resurfacing, and following radiation therapy. In rare cases, keratoacanthomas may develop as part of a syndrome.
- In Ferguson-Smith syndrome, patients develop multiple self-healing keratoacanthomas. It is often seen in younger individuals. It is a genetic condition inherited in an autosomal dominant manner.
- In generalized eruptive keratoacanthomas of Grzybowski, patients develop hundreds to thousands of keratoacanthomas on both the skin and mucous membranes. These keratoacanthomas are frequently chronic and progressive.
- In Muir-Torre syndrome, patients may develop keratoacanthomas along with sebaceous neoplasms and/or gastrointestinal or genitourinary malignancy.
- In familial keratoacanthomas of Witten and Zak, patients develop multiple large and small keratoacanthomas; it is inherited in an autosomal dominant fashion.



 Patient Information for
Patient Information for