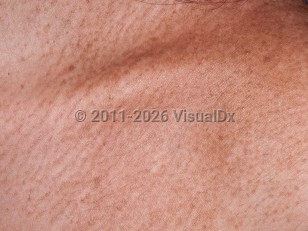
Macular amyloidosis
Alerts and Notices
Important News & Links
Synopsis

Macular amyloidosis (MA) is a form of primary cutaneous amyloidosis (a category which also includes lichen and nodular amyloidosis, poikiloderma-like cutaneous amyloidosis, primary cutaneous amyloidosis of the auricular concha, and the exceedingly rare entity of amyloidosis cutis dyschromica). In MA, a proteinaceous material, amyloid, which is derived from keratinocytes, is deposited in the superficial dermis without involvement of other tissue.
While the cause of MA is incompletely understood, it is associated with, and probably caused by, friction and scratching with fingernails or implements such as towels or brushes.
Clinically, MA manifests as hyperpigmentation. The most common locations are the upper back and extensor upper extremities. A rippled pattern is sometimes seen. MA and lichen amyloidosis (LA) are believed to exist on a spectrum and are mainly differentiated by the nature of the primary lesion (macules and patches in MA and thin plaques in LA) and histopathologic findings. Some patients also display features of both MA and LA, which is termed "biphasic amyloidosis."
MA is generally a pruritic condition, but it may sometimes be asymptomatic. MA has been described in the setting of connective tissue diseases, primary biliary cholangitis, and multiple endocrine neoplasia type 2a.
While the cause of MA is incompletely understood, it is associated with, and probably caused by, friction and scratching with fingernails or implements such as towels or brushes.
Clinically, MA manifests as hyperpigmentation. The most common locations are the upper back and extensor upper extremities. A rippled pattern is sometimes seen. MA and lichen amyloidosis (LA) are believed to exist on a spectrum and are mainly differentiated by the nature of the primary lesion (macules and patches in MA and thin plaques in LA) and histopathologic findings. Some patients also display features of both MA and LA, which is termed "biphasic amyloidosis."
MA is generally a pruritic condition, but it may sometimes be asymptomatic. MA has been described in the setting of connective tissue diseases, primary biliary cholangitis, and multiple endocrine neoplasia type 2a.
Codes
ICD10CM:
E85.9 – Amyloidosis, unspecified
SNOMEDCT:
111032003 – Macular cutaneous amyloidosis
E85.9 – Amyloidosis, unspecified
SNOMEDCT:
111032003 – Macular cutaneous amyloidosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:01/05/2020
Last Updated:05/11/2020
Last Updated:05/11/2020
Macular amyloidosis