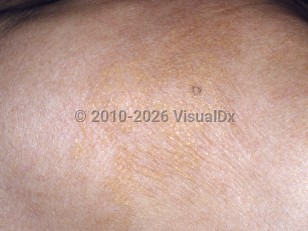
Plane xanthomas
Alerts and Notices
Important News & Links
Synopsis

Plane (planar) xanthomas are circumscribed or diffuse, yellow / orange macules, patches, or plaques that may occur in limited anatomical areas or may be more generalized. Areas of predilection include the eyelids (xanthelasma palpebrarum [XP]), lateral face and neck, upper torso including the shoulders, flexural areas, interdigital areas, and palms.
Over 50% of cases are due to an underlying lipid abnormality: hyperlipoproteinemia from primary metabolic lipoprotein abnormalities, such as familial hypercholesterolemia (type IIa hyperlipoproteinemia) or familial dysbetalipoproteinemia (type III hyperlipoproteinemia), or secondary causes of hyperlipidemia, such as hepatic cholestasis (eg, biliary atresia, primary biliary cirrhosis), may be associated. Xanthoma striatum palmare is strongly indicative of familial dysbetalipoproteinemia, and interdigital xanthomas strongly suggest the diagnosis of homozygous familial hypercholesterolemia. The quantitative or qualitative abnormality in serum lipid levels results in aggregation of lipoproteins that are phagocytosed by scavenger macrophages, forming foam cells that coalesce into plane xanthomas.
XP is the most commonly encountered type of xanthoma and is classified as a type of localized plane xanthoma. XP is associated with an underlying lipid abnormality in only around half of cases.
Other normolipemic plane xanthomas are less common and may be associated with paraproteinemias, most commonly multiple myeloma. Other associated diseases include monoclonal gammopathy of undetermined significance (MGUS), Waldenström macroglobulinemia, leukemia, lymphoma, cryoglobulinemia, Sézary syndrome, and Castleman disease. It is hypothesized that excess serum proteins bind lipoproteins to form modified lipoprotein complexes that are deposited in the skin and phagocytosed by scavenger macrophages, leading to foam cells and xanthoma formation.
Plane xanthomas tend to manifest in the fourth to fifth decade of life. They may rarely present in younger age groups, and when they do, they are almost always associated with a lipid abnormality. Familial hypercholesterolemia is the most common presenting primary dyslipidemia in this age group.
Over 50% of cases are due to an underlying lipid abnormality: hyperlipoproteinemia from primary metabolic lipoprotein abnormalities, such as familial hypercholesterolemia (type IIa hyperlipoproteinemia) or familial dysbetalipoproteinemia (type III hyperlipoproteinemia), or secondary causes of hyperlipidemia, such as hepatic cholestasis (eg, biliary atresia, primary biliary cirrhosis), may be associated. Xanthoma striatum palmare is strongly indicative of familial dysbetalipoproteinemia, and interdigital xanthomas strongly suggest the diagnosis of homozygous familial hypercholesterolemia. The quantitative or qualitative abnormality in serum lipid levels results in aggregation of lipoproteins that are phagocytosed by scavenger macrophages, forming foam cells that coalesce into plane xanthomas.
XP is the most commonly encountered type of xanthoma and is classified as a type of localized plane xanthoma. XP is associated with an underlying lipid abnormality in only around half of cases.
Other normolipemic plane xanthomas are less common and may be associated with paraproteinemias, most commonly multiple myeloma. Other associated diseases include monoclonal gammopathy of undetermined significance (MGUS), Waldenström macroglobulinemia, leukemia, lymphoma, cryoglobulinemia, Sézary syndrome, and Castleman disease. It is hypothesized that excess serum proteins bind lipoproteins to form modified lipoprotein complexes that are deposited in the skin and phagocytosed by scavenger macrophages, leading to foam cells and xanthoma formation.
Plane xanthomas tend to manifest in the fourth to fifth decade of life. They may rarely present in younger age groups, and when they do, they are almost always associated with a lipid abnormality. Familial hypercholesterolemia is the most common presenting primary dyslipidemia in this age group.
Codes
ICD10CM:
R23.8 – Other skin changes
SNOMEDCT:
238953008 – Plane xanthoma
R23.8 – Other skin changes
SNOMEDCT:
238953008 – Plane xanthoma
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:11/18/2020
Last Updated:12/02/2020
Last Updated:12/02/2020
Plane xanthomas