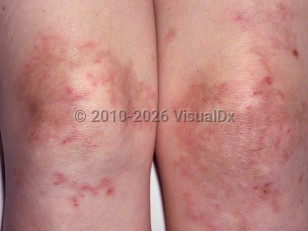
Polyarteritis nodosa in Adult
Alerts and Notices
Important News & Links
Synopsis

PAN most commonly involves the skin, peripheral nerves, kidneys, joints, and gastrointestinal tract. Any organ may be affected, although the lungs are typically spared. Constitutional symptoms may include malaise, fever, weakness, myalgias, arthralgias, and weight loss in combination with multiorgan symptoms of ischemia or infarction such as abdominal pain, cutaneous ulcers, livedo reticularis, testicular pain, mononeuropathy multiplex, and hypertension. Neurologic manifestations with asymmetric peripheral neuropathy can result in motor and sensory deficits and are the most common presenting organ manifestation. Renal involvement is common, manifested by hypertension and renal impairment, but red cell casts are notably absent; their presence should raise suspicion for an alternative diagnosis. Cardiac involvement presenting with myocardial infarction has been described. Other complications include stroke, gangrene, renal failure (acute, chronic), bowel ischemia and perforation, gastrointestinal bleeding, retinal detachment, and death. Corticosteroids and immunosuppressive medications are the cornerstones of treatment.
PAN usually affects individuals in the fourth to sixth decades of life. It is slightly more common in men, and there is no apparent racial predilection. An isolated cutaneous form also exists (cutaneous polyarteritis nodosa [cPAN]), which is more common in children. PAN has been most commonly associated with infection with hepatitis B (30% of patients are positive for the B antigen). There are reports of associations with hepatitis C, cytomegalovirus (CMV), parvovirus B19, human T-lymphotropic virus (HTLV type 1, type 2), and streptococci. There appears to be an association with inflammatory bowel disease (Crohn disease, ulcerative colitis). Minocycline has rarely been reported to induce both systemic PAN and limited cPAN.
Childhood-onset polyarteritis nodosa is a finding in deficiency of adenosine deaminase type 2 (DADA2), a rare multisystem vasculopathic syndrome due to autosomal recessive mutations in the CECR1 gene.
Codes
M30.0 – Polyarteritis nodosa
SNOMEDCT:
155441006 – Polyarteritis nodosa
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/25/2025