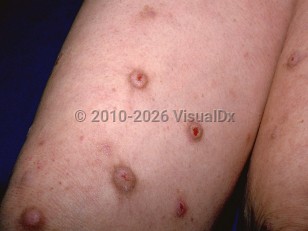
Prurigo nodularis in Child
Alerts and Notices
Important News & Links
Synopsis

Prurigo nodularis is a chronic condition that is triggered by repetitive rubbing or scratching of discrete areas of the skin. It may alternatively be induced by repetitive picking or rubbing of nonpruritic skin. Although the exact prevalence is unknown, it is most commonly seen in individuals aged 45 years and older and seems to be more common in women. It can rarely occur in children and teenagers, often in association with atopic dermatitis.
Prurigo nodularis presents as one or more (usually multiple) discrete, severely pruritic nodules that mostly appear on the extensor surfaces of extremities and anterior areas of the thighs and legs. The lesions are rarely seen on the face. Pruritus is described as severe and distressing and can become worse with heat, sweating, or irritation from friction.
Prurigo nodularis may be secondary to skin conditions associated with pruritus, such as atopic dermatitis and xerosis, as well as systemic conditions associated with generalized pruritus without a primary skin rash, such as HIV infection, iron deficiency anemia, diabetes mellitus (type 1, type 2), gluten enteropathy, thyroid disease, renal or hepatic impairment, malignancies, and others. In most cases, the etiology of pruritus is unknown. Studies have suggested that prurigo nodularis may be a form of subclinical small fiber neuropathy and that Th2 cytokines play an important role in its pathogenesis. In the nonpruritic cases, repetitive picking induces the lesions. In these cases, there may be an underlying psychological component that results in the inability to break the itch-scratch cycle.
Patients with this disorder may have an increased risk of various general medical conditions.
Prurigo nodularis presents as one or more (usually multiple) discrete, severely pruritic nodules that mostly appear on the extensor surfaces of extremities and anterior areas of the thighs and legs. The lesions are rarely seen on the face. Pruritus is described as severe and distressing and can become worse with heat, sweating, or irritation from friction.
Prurigo nodularis may be secondary to skin conditions associated with pruritus, such as atopic dermatitis and xerosis, as well as systemic conditions associated with generalized pruritus without a primary skin rash, such as HIV infection, iron deficiency anemia, diabetes mellitus (type 1, type 2), gluten enteropathy, thyroid disease, renal or hepatic impairment, malignancies, and others. In most cases, the etiology of pruritus is unknown. Studies have suggested that prurigo nodularis may be a form of subclinical small fiber neuropathy and that Th2 cytokines play an important role in its pathogenesis. In the nonpruritic cases, repetitive picking induces the lesions. In these cases, there may be an underlying psychological component that results in the inability to break the itch-scratch cycle.
Patients with this disorder may have an increased risk of various general medical conditions.
Codes
ICD10CM:
L28.1 – Prurigo nodularis
SNOMEDCT:
63501000 – Prurigo nodularis
L28.1 – Prurigo nodularis
SNOMEDCT:
63501000 – Prurigo nodularis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

To perform a comparison, select diagnoses from the classic differential
Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Reviewed:05/25/2025
Last Updated:05/26/2025
Last Updated:05/26/2025
 Patient Information for Prurigo nodularis in Child
Patient Information for Prurigo nodularis in Child
Premium Feature
VisualDx Patient Handouts
Available in the Elite package
- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient
Upgrade Today

Prurigo nodularis in Child