- Small vessel vasculitides include leukocytoclastic vasculitis (LCV), urticarial vasculitis, immunoglobulin A (IgA) vasculitis, and erythema elevatum diutinum (EED). Types II and III cryoglobulinemia also lead to a small vessel vasculitis. The ANCA-associated vasculitides include granulomatosis with polyangiitis (GPA), eosinophilic granulomatosis with polyangiitis (EGPA), and microscopic polyangiitis.
- Medium vessel vasculitides include polyarteritis nodosa (PAN) and Kawasaki disease.
- Large vessel vasculitides include Takayasu arteritis and giant cell (temporal) arteritis.
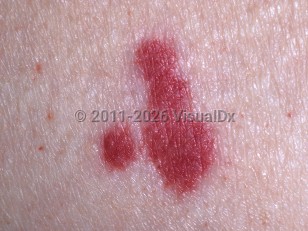
LCV is a histopathologic term that refers to inflammation of small blood vessels, usually with an inflammatory infiltrate and necrosis of the vessel wall. This form of vasculitis may be localized to the skin, where it is most commonly seen as palpable purpura, or it may also involve other organs such as the kidneys, joints, or gastrointestinal (GI) tract.
Urticarial vasculitis is a variant of LCV. It may be idiopathic, or it can occur in association with serum sickness, connective tissue disorders, infections, and from potassium iodide or NSAIDs. Urticarial plaques last longer than 24 hours.
EED refers to a rare subtype of LCV. It is associated with upper respiratory infections (especially streptococcal), HIV, hematologic disease, and rheumatologic disorders. It presents with arthralgias and erythematous-to-violaceous papules, plaques, and nodules with a predilection for extensor surfaces.
GPA is a multisystem disease characterized by vasculitis and necrotizing granulomatous inflammation of the small arteries and veins.
EGPA affects multiple body systems and is characterized by asthma, chronic rhinosinusitis, peripheral eosinophilia, and systemic small-to-medium vessel vasculitis.
PAN most commonly involves the skin, peripheral nerves, kidneys, joints, and GI tract. Symptoms may include malaise, fever (in 50% of cases), weakness, myalgias, arthralgias, abdominal pain, testicular pain, and weight loss. It has been associated with infection with hepatitis B, hepatitis C, HIV, cytomegalovirus (CMV), parvovirus B19, human T-cell lymphotropic virus (HTLV), and streptococci.
Drug-induced vasculitides are frequently ANCA-positive. They may present with skin involvement and, if progressive, can lead to glomerulonephritis, pulmonary hemorrhage, mononeuritis multiplex, and other complications of end-organ involvement. Onset of the vasculitis is variable, ranging from weeks to years after starting therapy. Hydralazine, propylthiouracil, carbimazole, minocycline, penicillamine, allopurinol, mirabegron, rifampicin, rosuvastatin, montelukast, the influenza vaccine, and pegylated interferon-alpha are frequent offenders.
Isotretinoin has been reported to induce vasculitis, sometimes with renal involvement. Levamisole, a veterinary medication banned for human use, has been shown to cause vasculitis. Cocaine contaminated with levamisole is a near-epidemic occurrence in cocaine users, leading to cocaine levamisole toxicity.