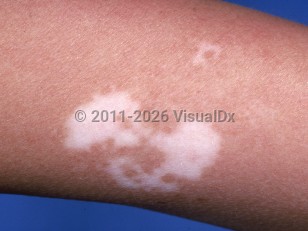
Vitiligo - Anogenital in
See also in: Overview,External and Internal EyeAlerts and Notices
Important News & Links
Synopsis

Two main clinical categories exist: segmental vitiligo and nonsegmental vitiligo.
In segmental vitiligo, depigmentation is usually seen unilaterally in a dermatomal or blaschkoid distribution.
Nonsegmental vitiligo is an umbrella term that encompasses most other patterns of vitiligo. It can affect any part of the body, but it often involves the face, upper chest, hands, ankles, axillae, groin, and around orifices (eyes, nose, mouth, urethra, and anus), favoring sites of frequent friction or trauma. Distinct patterns include acrofacial involvement (distal extremities and face), mucosal involvement (multiple mucosal sites, eg, both oral and genital involvement), generalized (widely distributed), and universal vitiligo (close to 100% of body surface area involved). Nonsegmental vitiligo may coexist with segmental vitiligo.
Anogenital involvement can be seen in both segmental and nonsegmental vitiligo; however, it is most common in nonsegmental types in the context of generalized disease. Less often, anogenital lesions in nonsegmental vitiligo present together with other affected mucosal sites. Very rarely, a small anogenital lesion can occur in isolation.
Overall, vitiligo occurs in equal proportions regardless of sex or race / ethnicity. There is a bimodal pattern of onset, first in childhood and then in adulthood. The adult-onset population accounts for approximately two-thirds of cases and has a mean onset of 34 years. The natural progression of the disease is unpredictable, ranging from insidious to rapid in onset. Years of stable, nonprogressive disease can be observed with the disease subsequently taking an unexpected rapid trajectory. Approximately one-third of patients with vitiligo report anogenital involvement, regardless of race / ethnicity. The presence of anogenital lesions may be slightly higher in males.
While the precise etiology of vitiligo remains debated, the leading hypothesis implicates both genetic and environmental factors that lead to an innate immune response resulting in CD8+ T-cell activation, release of interferon-γ (IFN-γ), and an associated inflammatory cascade in keratinocytes via the JAK/STAT pathway.
Environmental factors include mechanical trauma and/or exposure to depigmenting agents.
While most vitiligo patients are otherwise healthy, an association with autoimmune thyroid dysfunction (hyperthyroidism or hypothyroidism) has been demonstrated. In new-onset vitiligo patients with systemic symptoms, thyroid screening with antithyroid peroxidase (TPO) antibody and a serum thyrotropin is recommended. Additional associations include endocrinopathies, such as diabetes mellitus (type 1, type 2) and Addison disease, along with other autoimmune processes. Rarely, it may exist as part of polyglandular autoimmune syndrome, particularly a type III syndrome (eg, Hashimoto thyroiditis, vitiligo, or alopecia areata and/or another organ-specific autoimmune disease). Vitiligo may accompany halo nevi. New-onset vitiligo may be seen in patients with metastatic melanoma. It can occur spontaneously and may herald metastatic disease, or it can be triggered by immunotherapy such as with BRAF inhibitors or PD-1 inhibitors. In the latter setting, it is considered a good prognostic sign. Rarely, vitiligo may be associated with uveitis. An increased risk of developing sensorineural hearing loss has been identified in both adults and children with vitiligo.
Related topic: segmental vitiligo
Codes
L80 – Vitiligo
SNOMEDCT:
56727007 – Vitiligo
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:06/22/2025
 Patient Information for Vitiligo - Anogenital in
Patient Information for Vitiligo - Anogenital in - Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient