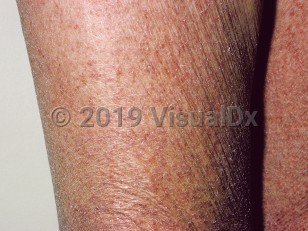
Acquired ichthyosis in Child
Alerts and Notices
Important News & Links
Synopsis

AI may be associated with underlying malignancies, infectious, inflammatory, or metabolic disorders, or with medications. The most common associated malignancy is Hodgkin disease. Other less frequent associations include multiple myeloma, cutaneous T-cell lymphoma and other lymphoproliferative disorders, leiomyosarcoma, Kaposi sarcoma, and carcinomas of the breast, lung, liver, and bladder. Skin changes are most often noted following the diagnosis of the malignancy.
AI is often seen in human immunodeficiency virus (HIV) infection, usually with a low CD4+ count, and not necessarily associated with malignancy. It has also been reported in the setting of active tuberculosis infection.
Acquired ichthyosis may be seen with chronic metabolic disturbances (malnutrition, malabsorption, renal failure, hyperparathyroidism, hypopituitarism, hypothyroidism, and diabetes). It also occurs on occasion with connective tissue disease (eg, systemic lupus and dermatomyositis) as well as with sarcoidosis, Hansen disease (leprosy), and post-bone marrow transplant.
Drug-induced acquired ichthyosis may be caused by cholesterol-lowering agents, isoniazid, acitretin, butyrophenones, dixyrazine, maprotiline, cimetidine, allopurinol, hydroxyurea, and clofazimine.
Coincident hair loss may occur, as may pruritus or a burning sensation. Symptoms usually improve in a warm, moist climate.
Disease severity may parallel the course of the associated disorder. Acquired ichthyosis often remits after treatment of underlying malignancy.
Codes
L85.0 – Acquired ichthyosis
SNOMEDCT:
8691004 – Acquired ichthyosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:09/15/2019
 Patient Information for Acquired ichthyosis in Child
Patient Information for Acquired ichthyosis in Child- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient