Psoriasis is a polygenic disease. (Several psoriasis susceptibility genes have been identified over recent years.) Certain individuals with genetic susceptibility develop a psoriatic phenotype after exposure to environmental triggers such as infection, medications, and medical comorbidities, among others. Aberrant T-cell function and keratinocyte responses are believed to be major culprits in the pathogenesis of psoriasis.
There are several variants of the disease, and variants can coexist in the same individual.
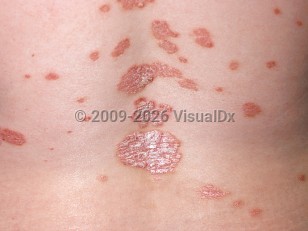
Chronic plaque psoriasis is most common, and disease burden can range from 1%-2% (mild disease) to greater than 90% (erythrodermic psoriasis) of the total body surface area (BSA). Typical findings include well-demarcated circular, oval, or polycyclic erythematous plaques with micaceous scale that are often symmetric in distribution. The scalp, elbows, and knees are commonly involved. Lesions are often pruritic and resolve with postinflammatory hyper- or hypopigmentation. Scarring is not a feature of resolution. During exacerbations, erythematous papules usually surround existing plaques, and a ring of intense erythema surrounds the plaques. During resolution, plaques will often have a decreased amount of scale and central clearing, creating annular psoriatic lesions. Lesions can last from months to years in the same location.
When psoriasis involves areas of the face other than the hairline, eyebrows, and beard, it is usually an indication of more severe disease. Seborrheic dermatitis can coexist with psoriasis on the face and scalp (sometimes referred to as "sebopsoriasis").
Variants include:
- Psoriatic arthritis – Up to 50% of psoriatic individuals may have erosive psoriatic arthritis. Psoriatic arthritis is more common among individuals with nail and scalp psoriasis. Rarely, psoriatic arthritis has been reported to develop prior to the cutaneous findings of psoriasis.
- Guttate psoriasis – An acute generalized eruption of small, discrete, raindrop-like papules with fine scale. This may occur 2-3 weeks after an upper respiratory infection and is most common in children.
- Erythrodermic psoriasis – An uncommon but potentially life-threatening acute complication of psoriasis wherein large red patches with desquamation cover most of the body surface.
- Pustular psoriasis – An uncommon, sometimes severe, variant characterized by widespread erythematous, sterile pustules.
- Acrodermatitis continua of Hallopeau – An uncommon variant of pustular psoriasis affecting the hands and feet.
- Inverse psoriasis – Psoriasis that involves the intertriginous areas including the axillae, inframammary areas, and inguinal folds. The plaques of inverse psoriasis are erythematous and well-demarcated but often lack the classic scale as these body sites are generally moist.
- Nail psoriasis – The nails of individuals with psoriasis can show several features. The most common are pitting, distal onycholysis, and splinter hemorrhages. Individuals with nail psoriasis are at an increased risk of developing psoriatic arthritis.
Approximately 50% of women report improvement of disease burden during pregnancy. Pustular psoriasis developing in hypocalcemic women during pregnancy is known as pustular psoriasis of pregnancy, or impetigo herpetiformis.
HIV infection may precipitate or exacerbate psoriasis.



 Patient Information for
Patient Information for