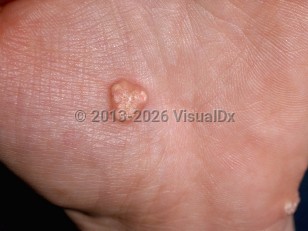
Calcinosis cutis in Adult
Alerts and Notices
Important News & Links
Synopsis

The most common clinical presentation is that of irregularly surfaced papules, nodules, and plaques. Extrusion of a chalk-like substance from calcified nodules and secondary infection can cause pain and significant morbidity.
Disorders of calcium deposition can be broadly categorized into 5 main subtypes: dystrophic, metastatic, mixed, idiopathic, and iatrogenic.
Dystrophic calcinosis cutis occurs when calcium is deposited in previously damaged skin in the absence of abnormal serum calcium and phosphorus levels. Dystrophic calcinosis cutis in adults is often seen in autoimmune connective tissue diseases, especially in the CREST form of systemic sclerosis. It is also seen in juvenile dermatomyositis and occasionally in adult dermatomyositis (10%-20%). Less often, it can be seen in acute systemic lupus erythematosus, subacute cutaneous lupus erythematosus, chronic cutaneous lupus erythematosus, lupus panniculitis, and generalized morphea. Other causes include trauma, scarring (eg, in acne vulgaris), neoplasms (eg, calcified cysts, pilomatricoma, melanocytic nevi, basal cell carcinomas, desmoplastic trichoepitheliomas, chondroid syringomas), genodermatoses (eg, pseudoxanthoma elasticum, Werner syndrome, Ehlers-Danlos syndromes) and infection (eg, onchocerciasis, cysticercosis, histoplasmosis, cryptococcosis).
Calcinosis universalis refers to the most severe form of dystrophic calcification. Usually observed in the setting of dermatomyositis or other connective tissue diseases such as systemic lupus erythematosus, this variant involves extensive areas of cutaneous calcification in sheet-like masses and can cause severe functional impairment.
Metastatic calcinosis cutis occurs when calcium deposits occur in the setting of systemic metabolic disorders with calcium and/or phosphorus imbalance. The most common cause of metastatic calcinosis cutis is advanced renal disease. Other causes include hypervitaminosis D, milk-alkali syndrome, Albright hereditary osteodystrophy (pseudohypoparathyroidism type 1A), hyperparathyroidism, malignancy, and sarcoidosis.
The mixed type refers to the presence of both dystrophic and metastatic forms.
Idiopathic calcinosis cutis includes scrotal calcinosis (idiopathic calcification of the scrotum), subepidermal calcified nodule, and tumoral calcinosis. Scrotal calcinosis occurs on the scrotum of otherwise healthy males and presents with nontender, white or yellow, hard papules and nodules. This condition has been thought by some to represent calcified epidermal inclusion cysts. Subepidermal calcified nodule presents as a solitary hard white papule or nodule on the head (often the ear), neck, or upper extremities in children. Tumoral calcinosis presents as large nodules on periarticular locations in healthy adolescents.
Iatrogenic calcinosis cutis occurs in temporal relation to administration of intravenous calcium gluconate, calcium chloride, or para-aminosalicylic acid (for treatment of pulmonary tuberculosi), at sites of application of calcium alginate dressings to denuded skin or calcium chloride-containing electrodes used for electroencephalography.
Codes
L94.2 – Calcinosis cutis
SNOMEDCT:
21323007 – Calcinosis cutis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:05/31/2020